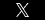Search
Government Report Confirms Pressure Ulcers Harm All Nursing Home Residents; Regardless Of Race, Sex or Age
A report released by the Centers for Disease Control and Prevention confirmed what many nursing home residents and employees already know– pressure ulcers are a tremendous problem encountered be nursing home residents of all races, sexes and ages. The report,“Pressure Ulcers Among Nursing Home Resident: United States, 2004” analyzes information from the National Nursing Home Survey which is comprised of more than 14,000 nursing home residents from across the country.
 In 2004, more than one in 10 nursing home residents had some form of pressure ulcer within the year. Based on the total number of nursing home residents, that translates to more than 159,000 nursing home residents with pressure ulcers (otherwise known as bed sores, decubitus ulcers, or pressure sores). Stage II pressure ulcers were the most common according to the survey. Over 35% of the nursing home residents with pressure ulcers had more advanced– stage III or stage IV ulcers that required special wound treatment. Even younger nursing home residents, those commonly thought to be somewhat removed from the problem, are at risk according to the report.
In 2004, more than one in 10 nursing home residents had some form of pressure ulcer within the year. Based on the total number of nursing home residents, that translates to more than 159,000 nursing home residents with pressure ulcers (otherwise known as bed sores, decubitus ulcers, or pressure sores). Stage II pressure ulcers were the most common according to the survey. Over 35% of the nursing home residents with pressure ulcers had more advanced– stage III or stage IV ulcers that required special wound treatment. Even younger nursing home residents, those commonly thought to be somewhat removed from the problem, are at risk according to the report.
The study demonstrates that while it is important to identify nursing home residents who are at risk for development of pressure ulcers and implement preventative techniques, no nursing home resident is immune from risk of developing pressure ulcers and the nursing home staff need to be tuned in to the factors related to pressure ulcer development and treatment.
About Pressure Ulcers
A pressure ulcer is an area of skin that breaks down when you stay in one position for too long without shifting your weight. This often happens if you use a wheelchair or you are bedridden, even for a short period of time (for example, after surgery or an injury). The constant pressure against the skin reduces the blood supply to that area, and the affected tissue dies.
A pressure ulcer starts as reddened skin but gets progressively worse, forming a blister, then an open sore, and finally a crater. The most common places for pressure ulcers are over bony areas like the elbow, heels, hips, ankles, shoulders, back, and the back of the head.
Despite claims from the health care industry, pressure ulcers are preventable with competent medical care. Staff in nursing homes and hospitals must to an assessment of those individuals who are at heightened risk for development of pressure ulcers and development a plan for their care. Frequently, a care plan will include: frequent rotation to discourage sitting in one area for long periods, pressure relieving air mattresses and special high nutrition diets.
Factors increasing the risk for development of pressure ulcers:
- Being bedridden or in a wheelchair
- Fragile skin
- Having a chronic condition, such as diabetes or vascular disease, that prevents areas of the body from receiving proper blood flow
- Inability to move certain parts of your body without assistance, such as after spinal or brain injury or if you have a neuromuscular disease (like multiple sclerosis)
- Malnourishment
- Mental disability from conditions such as Alzheimer’s disease — the patient may not be able to properly prevent or treat pressure ulcers
- Older age
- Urinary incontinence or bowel incontinence
Pressure sores are categorized by severity, from Stage I (earliest signs) to Stage IV (worst):
- Stage I: A reddened area on the skin that, when pressed, is “non-blanchable” (does not turn white). This indicates that a pressure ulcer is starting to develop.
- Stage II: The skin blisters or forms an open sore. The area around the sore may be red and irritated.
- Stage III: The skin breakdown now looks like a crater where there is damage to the tissue below the skin.
- Stage IV: The pressure ulcer has become so deep that there is damage to the muscle and bone, and sometimes tendons and joints.
Web Resources For Information On Pressure Ulcers:
National Pressure Ulcer Advisory Panel
Staging Pressure Ulcers, Wound Care Information Network
// //
 Nursing Home Law News
Nursing Home Law News