The Nursing Home Law Center is committed to providing the legal resources necessary to hold negligent facilities accountable.
New Mexico Nursing Home Abuse Lawyer

Licensed in New Mexico
Nursing home residents, many of whom are vulnerable elderly individuals, rely on nursing home residencies to provide proper care and a safe environment. Unfortunately, some nursing homes fail to meet this responsibility, leading to cases of nursing home abuse and neglect.
In these situations, it’s important to seek help from an experienced New Mexico nursing home abuse lawyer. With the legal guidance of a nursing home abuse attorney, families can seek justice and compensation for the harm caused to their loved ones. Legal support is particularly critical in large urban centers where facilities often face staffing challenges. If you are dealing with a claim in Bernalillo County, an Albuquerque Nursing Home Abuse Lawyer can help you navigate the local court system and hold negligent care providers accountable for their failures.
Why Hire Nursing Home Law Center
At Nursing Home Law Center, we are dedicated to ensuring justice and obtaining compensation for those harmed by elder abuse. Our skilled legal team has a strong history of successfully handling abuse cases, delivering favorable outcomes through settlements and verdicts.
We take a comprehensive approach in our investigations, ensuring that every aspect of the abuse is addressed, including medical costs, emotional suffering, and other associated damages. With our extensive knowledge of nursing home negligence claims, we effectively manage the legal challenges while relentlessly working to defend your rights.
Throughout the entire process, we offer compassionate, clear communication, making sure that you and your loved one feel supported, informed, and confident with each step forward.
Types of Cases Handled by Our New Mexico Nursing Home Abuse Lawyers
Elder abuse refers to any intentional harm or neglect inflicted on residents in nursing home residencies. This abuse can take many forms, and each case requires careful legal examination to hold responsible parties accountable.
Our experienced nursing home abuse lawyers handle a wide range of abuse cases, ensuring victims receive justice and compensation for their suffering.
Physical Abuse
Physical abuse involves intentional harm such as hitting, slapping, or pushing a nursing home resident. It also includes the improper use of restraints or force, leading to physical injuries such as broken bones, bruises, or other serious harm. When these incidents occur in Southern New Mexico, families must act to secure the safety of their relatives. A dedicated Las Cruces Nursing Home Abuse Lawyer will investigate the facility’s history of safety violations and work to recover damages for injuries caused by staff misconduct.
Mental and Emotional Abuse
Mental and emotional abuse can be just as damaging as physical abuse. This includes verbal threats, humiliation, intimidation, or isolation that causes emotional trauma to the resident, resulting in mental distress, anxiety, or depression.
Sexual Abuse
Sexual abuse in nursing homes involves any unwanted sexual contact or advances made toward a resident. This form of abuse can leave lasting emotional and physical scars, particularly for vulnerable elderly individuals unable to defend themselves.
Medical Malpractice
Medical malpractice in nursing homes can manifest through severe neglect, such as the development of bedsores, medication errors, or failure to provide appropriate medical care. This can lead to serious health complications, infections, or even wrongful death.
Negligence
Negligence is a common form of abuse in nursing homes. It can include poor hygiene practices, malnutrition, dehydration, or even elopement, where a resident wanders away from the assisted living facility unsupervised. Addressing these failures in Sandoval County requires a thorough investigation into operational standards. For families who suspect mistreatment, consulting a Rio Rancho Nursing Home Abuse Lawyer is a decisive step toward securing the evidence needed to prove life-altering neglect.
Financial Abuse
Financial abuse occurs when a staff member or another person takes advantage of a resident’s financial resources without their consent. This can involve theft, fraud, or manipulation, leaving the victim and their family with financial losses. Protecting the assets of vulnerable seniors in Chaves County requires vigilant legal oversight. Working with a Roswell Nursing Home Abuse Lawyer ensures that suspicious transactions are investigated and that those responsible for exploiting residents are held legally and financially responsible.
Wrongful Death
In the most tragic cases, nursing home neglect or abuse can lead to wrongful death. When a nursing home’s negligence or abusive practices cause the death of a resident, their family may pursue legal action to seek justice and hold the assisted living facility accountable.

Understanding Your Legal Rights
Several federal and state laws protect nursing home residents, ensuring their safety, dignity, and well-being. These protections are crucial in preventing abuse and neglect and provide a clear path for legal action when nursing homes fail in their duty of care.
The Nursing Home Reform Act of 1987 was enacted to improve the quality of care in nursing homes across the country. This law establishes the right of nursing home residents to receive proper care, which includes freedom from abuse, neglect, and exploitation.
Under this act, nursing homes must provide services that promote their residents’ physical, mental, and social well-being. The law also guarantees residents the right to privacy, the right to participate in their own care decisions, and the right to live in a dignified environment.
In New Mexico, nursing home residents are further protected by state laws that enforce strict licensing requirements for nursing homes and establish guidelines for patient care. The New Mexico Department of Health oversees nursing home inspections and investigates complaints about poor conditions, neglect, or abuse.
New Mexico law ensures that residents have the right to quality care, be treated with respect, and live in an environment free from harm.
Eligibility to File a Nursing Home Abuse Claim in New Mexico
A nursing home negligence or abuse claim can be filed by the abused resident, or in cases where the resident is unable to do so, such as those with cognitive impairments or incapacitation, their legal guardian or a designated family member can file the claim on their behalf.
In the event of a wrongful death due to nursing home negligence or abuse, surviving family members may file a lawsuit seeking justice and compensation for their loss.

Liability in Nursing Home Neglect and Abuse Cases
In nursing home neglect and abuse cases, multiple parties can be held responsible for the harm inflicted on residents. Liability often extends beyond the individual perpetrator to other entities that failed to provide proper care and oversight. By identifying all responsible parties, victims and their families can pursue justice and seek full compensation for the damages.
- Nursing Home Facility: The nursing home can be held liable if it fails to implement adequate policies, training, or supervision of its staff. The facility may also be responsible for abuse or neglect if it allows understaffing or hires unqualified personnel, leading to inadequate patient care.
- Nursing Home Staff: Individual staff members, such as nurses, aides, or caregivers, can be personally liable if they directly inflict abuse or engage in neglectful behavior. Their failure to uphold the standard of care can result in legal action against them.
- Administrators and Supervisors: Nursing home administrators and supervisors may be liable if they fail to properly manage the facility, enforce safety protocols, or address reports of abuse. Their negligence in overseeing operations can contribute to an environment where abuse and neglect occur.
- Contractors and Third-Party Service Providers: Sometimes, nursing homes rely on third-party contractors for services like medical care, cleaning, or security. If these contractors contribute to abuse or neglect through their actions or inadequate services, they can be held accountable.
- Owners and Private Investors: Nursing home owners or private investors may be responsible if they prioritize profit over the well-being of residents. When cutting costs results in poor care or understaffing, owners can be legally liable for contributing to the abuse or neglect of residents.
- Physicians and Medical Staff: Medical professionals who provide care in nursing homes can be held accountable if they engage in medical malpractice, such as failing to diagnose or treat conditions, prescribing incorrect medications, or neglecting a patient’s medical needs.

How Our New Mexico Nursing Home Abuse Attorneys Can Help
At Nursing Home Law Center, our attorneys have extensive experience handling cases of nursing home abuse and neglect in New Mexico. We understand the emotional and physical toll these cases take on victims and their families, and we are committed to seeking justice for those harmed.
With a proven track record of securing significant settlements and verdicts, our legal team is prepared to fight for your rights every step of the way. Here’s how our dedicated New Mexico nursing home abuse lawyers can help:
Free Case Evaluation
We offer a free consultation to discuss your situation and evaluate the details of your case. During this evaluation, we listen carefully to understand the specifics of the abuse or neglect and advise you on the best course of legal action. This no-obligation meeting helps you make an informed decision about how to move forward with your claim.
Case Investigation
Once you decide to work with us, we thoroughly investigate the nursing home’s practices, staff members, and any incidents of abuse or neglect. Our personal injury attorneys gather evidence, review medical records, interview witnesses, and consult with experts to build a strong case. This investigation ensures that all aspects of the abuse, including physical injuries, emotional trauma, and medical expenses, are fully documented.
Filing the Claim
Our legal team will handle the complex process of filing a nursing home negligence claim on your behalf. We ensure all legal documents are filed correctly and within the required timelines. This step is crucial in protecting your right to seek compensation for the harm caused by nursing home negligence or abuse.
Settlement Negotiation
Many nursing home neglect and abuse cases are resolved through settlement negotiations. Our personal injury attorneys have extensive experience negotiating with nursing homes, insurance companies, and their legal teams to secure the maximum compensation for our clients.
We fight tirelessly to ensure that your family receives compensation for medical bills, emotional distress, and other damages caused by the abuse.
Trial Representation
We are fully prepared to take your case to trial if a fair settlement cannot be reached. Our trial lawyers deeply understand New Mexico nursing home laws and have successfully litigated numerous cases. We will present your case in court, advocating aggressively to ensure justice is served and those responsible for the abuse are held accountable.

Common Signs of Elder Abuse Among Nursing Home Residents
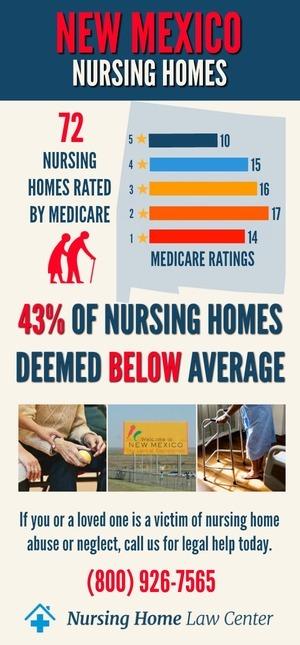
There are a total of 68 Medicare-approved nursing homes in New Mexico. Thirty-two of these facilities (47%) have an overall rating below or much below average. Specifically, 31 nursing homes (46%) fall short in health inspections, and 34 facilities (50%) have inadequate staffing. Fifteen facilities (22%) were rated poorly regarding quality measures. [1]
The worst-rated New Mexico nursing homes include:
| Bear Canyon Rehabilitation Center | Calibre Post Acute, LLC |
| Casa Arena Healthcare LLC | Casa DE Oro Center |
| Casa Maria Healthcare | Casa Real |
| Clovis Healthcare and Rehabilitation Center | Ladera Center |
| LA Vida Buena Healthcare | New Mexico State Veterans Home |
| Rio Rancho Center | Sandia Ridge Center |
| Skies Healthcare & Rehabilitation Center | Sunset Villa Healthcare |
| The Suites Rio Vista |
Recognizing the signs of nursing home abuse is critical in protecting the well-being of a nursing home resident. Abuse and neglect can take many forms, and some signs may be subtle or easily overlooked, especially if the victim is unable to communicate their suffering.
Families should stay vigilant and pay close attention to changes in their family member’s physical or emotional state. Here are some common signs of nursing home abuse that may indicate something is wrong:
- Unexplained Injuries
- Poor Hygiene
- Bedsores
- Sudden Weight Loss or Dehydration
- Emotional or Behavioral Changes
- Unexplained Fear or Anxiety
- Poor Living Conditions
- Financial Discrepancies
- Frequent Infections or Illnesses


What to Do If You Suspect Nursing Home Abuse
If you suspect that your family member is a victim of nursing home abuse, it is crucial to take immediate action to protect their safety and well-being. Here are the essential steps you should follow:
- Call 911 if there is immediate danger
- Report to the nursing home administrator or management
- File a complaint with your local ombudsman’s office
- Contact a nursing home abuse lawyer
Damages You Can Recover Through a Nursing Home Abuse Claim
Filing a nursing home abuse claim allows victims and their families to seek compensation for the harm caused.
Economic Damages
Economic damages compensate for the financial costs associated with the abuse or neglect. Examples include:
- Medical Expenses: This covers the cost of medical care related to the abuse or neglect, including hospital stays, doctor visits, physical therapy, medication, and any future medical treatments required.
- Relocation Costs: If the victim needs to be moved to a new facility due to the abuse, families can recover the expenses related to transferring the resident to a safer environment.
- Lost Financial Support: In some cases, the abuse or neglect may cause a financial strain on the victim’s family, such as if they had to leave work to care for their loved one. These losses can be compensated as part of economic damages.
Non-Economic Damages
Non-economic damages compensate for the more intangible losses that arise from nursing home abuse. Examples include:
- Pain and Suffering: Compensation for the pain and trauma the victim endured as a result of physical and emotional abuse.
- Emotional Distress: Nursing home abuse often leads to mental and emotional anguish, including anxiety, depression, and fear, which can be compensated through non-economic damages.
- Loss of Enjoyment of Life: If the abuse leads to a significant decline in the resident’s ability to enjoy daily activities or overall quality of life, this can be compensated under non-economic damages.
Punitive Damages
Punitive damages may be awarded in cases of particularly egregious abuse or neglect. Unlike economic and non-economic damages, designed to compensate the victim, punitive damages punish the wrongdoers and deter similar misconduct.

The Cost of Hiring a New Mexico Nursing Home Abuse Lawyer
At Nursing Home Law Center, we understand that financial concerns may be a worry when considering legal action. That’s why our New Mexico nursing home abuse lawyers work on a contingency fee basis. This means that you pay no upfront costs for our legal services, and we only collect a fee if we successfully recover compensation for you through a settlement or verdict.
You Have Limited Time to Take Legal Action in New Mexico
If you suspect that your loved one has suffered from nursing home negligence, it’s important to act quickly. In New Mexico, like all states, a statute of limitations restricts the amount of time you have to file a claim.
Generally, New Mexico law gives personal injury victims three years from the date of the abuse or injury to file a lawsuit. However, several factors in your case can influence the statute of limitations.
Failing to file within the statute of limitations could result in your case being dismissed, preventing you from seeking compensation for your loved one’s injuries.
An experienced New Mexico nursing home abuse lawyer can help you understand the specific timelines and ensure that your claim is filed on time so your family can seek justice.

Contact a New Mexico Nursing Home Abuse Lawyer Today!
At Nursing Home Law Center, we have extensive experience representing victims of nursing home abuse and neglect throughout New Mexico. Our dedicated team understands the pain and trauma these situations cause for families, and we are committed to helping you seek justice and full compensation for the harm done.
With a proven track record of securing favorable outcomes through settlements and verdicts, we provide the legal guidance and compassionate support you need during this difficult time.
Call us at (800) 926-7565 or fill out our contact form.
References: [1] Medicare

