The Nursing Home Law Center is committed to providing the legal resources necessary to hold negligent facilities accountable.
Can Bed Sores Lead to Death?
A bedsore can become fatal when the wound is allowed to deepen, become infected, and trigger complications such as sepsis, septic shock, or multi-organ failure. 42 C.F.R. § 483.25(b) requires the facility to provide care that prevents pressure ulcers unless they were clinically unavoidable, and to give residents the treatment needed to promote healing, as well as prevent infection and new ulcers from developing. When a facility ignores those duties and a resident dies from bedsore complications, a nursing home bedsore lawyer from our team can help.
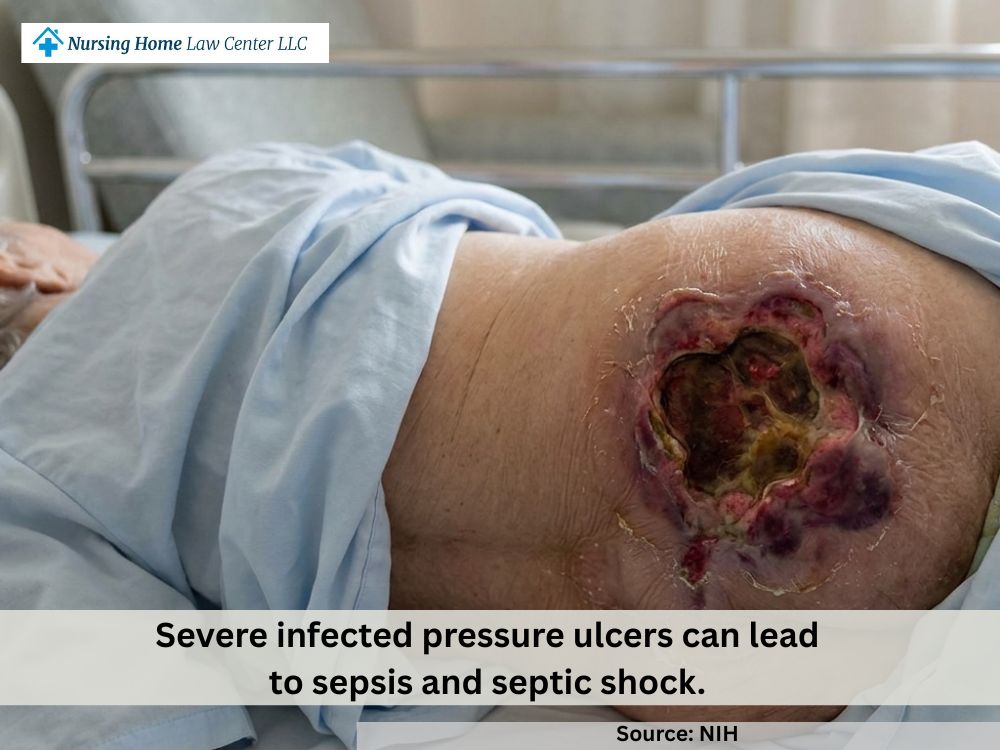
What Are Bed Sores?
Bed sores, also called pressure ulcers or decubitus ulcers, are wounds caused by prolonged pressure on the skin and underlying tissue. They usually develop when a person is unable to move enough to relieve pressure, especially over areas where they commonly occur, such as the heels, hips, tailbone, and elbows. In nursing home residents, they are often a sign that basic repositioning, skin monitoring, and daily care were not handled properly.
How Often Do Bedsores Lead to Death?
- Over 60,000 people die each year because of bedsore complications. (AHRQ)
- Nursing home residents with pressure ulcers experience a 6-month mortality rate of 77.3%, and 55.7% of those who die with a bedsore do so within 6 weeks of its onset. (HMP Global Learning Network)
- Individuals with pressure sores are 4.5X more at risk of death than those with the same risk factors but without pressure sores. (NCBI)
- Wound-related bacteria in the bloodstream can increase the risk of mortality to 55%. (Medscape)
How Do Pressure Ulcers Progress?
Pressure sores vary in severity.
Stage 1
During a stage 1 pressure sore, the skin’s outer layer will develop non-blanchable redness, meaning it does not turn white when pressed. The affected skin is still intact and may feel warm; more severe pressure ulcers may leave the skin purple or blue, and this early stage is more difficult to diagnose in people with darker skin.
Stage 2
Stage 2 decubitus ulcers will start to affect the integrity of the skin. The skin has partial thickness loss, which manifests as a partially open wound. These pressure injuries look like abrasions or blisters in the affected area. The skin itself will be discolored, and the surrounding skin will be painful.
Stage 3
Stage 3 pressure ulcers involve a lot of dead tissue, which means skin thickness loss is occurring. The sore will look like a crater, and the edges of the sore may have dark patches of dead tissue. There may also be necrosis in the subcutaneous tissue, which means the deep wound penetrates the fat layer.
Stage 4
Stage 4 pressure injuries involve full-thickness tissue loss, exposing bones, such as shoulder blades, tendons, or muscle tissue. The skin has been completely lost, creating serious risks of bacterial infection that can lead to death.
How Do Bedsores Become Fatal?
A bedsore becomes dangerous when the wound stops being a surface injury and turns into a systemic one. The process usually starts with skin breakdown, which creates an opening for bacteria to enter the tissue. From there, the bedsore infection can spread deeper into the muscle or bone, then move into the bloodstream. Once that happens, the resident may develop sepsis, then septic shock, followed by organ failure, and ultimately death.
What Are the Warning Signs a Bedsore Might Become Life-Threatening?
A bedsore may be becoming life-threatening when the wound starts showing signs of serious infection or the resident begins declining more broadly. Signs can include:
- foul odor,
- pus or drainage,
- fever,
- black tissue or necrosis,
- increasing redness or warmth around the wound.

What Causes Bedsores?
Pressure ulcers are caused by sustained pressure on the skin and underlying tissue, usually when a person is unable to move enough to relieve that pressure. Friction, shear, moisture, poor nutrition, dehydration, and reduced blood supply can make the damage worse. In nursing home residents, bed sores often develop when health care providers fail to reposition the resident, monitor the fragile skin, manage incontinence, or respond to early signs. Sadly, it is estimated that 11% of nursing home residents have pressure injuries. (CDC)
Where Do Pressure Sores Typically Appear?
Skin ulcers commonly develop in areas where bone and skin are in constant contact with a surface, such as:
- Tailbone and buttocks
- Shoulder blades and the back of the head
- Ankles and heels
- Hips and lower back
What Are the Risk Factors for Developing Bedsores?
Nursing home residents who are at a heightened risk of developing bedsores are bedridden patients, those who are immobile, or dependent on a wheelchair, especially if they need staff help to reposition. Risk also rises with advanced age, spinal cord injury, poor blood flow, limited oxygenation, kidney disease, malnutrition, dehydration, and other conditions that slow healing or weaken the body’s ability to fight infection.
How Can Nursing Homes Prevent Pressure Injuries?
To help prevent bedsores, nursing home staff should:
- Reposition residents regularly to reduce pressure on high-risk areas such as the heels, hips, tailbone, and ankles
- Use pressure-relieving mattresses, cushions, and other support surfaces when needed
- Check the skin daily for redness, breakdown, drainage, or other early warning signs
- Keep the skin’s surface dry, clean, and protected from excess moisture
- Manage incontinence promptly so moisture does not sit on the skin
- Make sure residents receive enough food, fluids, and protein to support healthy skin and wound healing
- Document changes quickly and start wound care before a minor pressure spot becomes a deep ulcer
- Send the resident for higher-level medical treatment when the wound shows signs of infection or rapid worsening
Can Bedsores Be Treated Before They Turn Fatal?
Pressure sores can and should be treated as early as possible, before a minor pressure spot turns into a deep wound or a life-threatening infection, including bone infection, joint infection, or worse. Bedsore treatment includes:
- Reducing pressure on the affected area by repositioning the resident more often and using pressure-relieving mattresses, cushions, or other supports to keep the wound from getting worse.
- Wound cleaning and dressing to reduce the risk of infection and support healing. In more serious cases, dead tissue may need to be removed (debridement) so the wound can be treated more effectively and the infection does not spread deeper into the body.
- Ensuring adequate fluids, protein, and overall nutritional support to help the skin recover and to reduce the risk of worsening complications.
- Infection treatment using antibiotics, and, in severe cases, hospital treatment for deeper infection, sepsis, or other systemic complications.
Why Fatal Bedsores Often Point to Nursing Home Neglect
Fatal bedsores often point to neglect because they are usually tied to failures in basic care. With proper care, bedsores are preventable injuries. Bedsores in nursing homes often develop when staff fail to reposition residents, neglect nutritional needs, fail to keep the skin clean and dry, or fail to monitor and treat bedsores.

That is why a fatal bedsore case usually raises a larger negligence question. Our attorneys are looking at whether the home missed skin assessments, delayed wound care, ignored hydration or nutrition problems, failed to offload pressure, or waited too long to send the resident out for proper treatment after the ulcer became infected. We’re also looking at systemic issues such as understaffing, which is often where the pattern starts.
The facility may be held liable if a nursing home resident dies after they were known to be at risk, the ulcer was preventable, and the staff still let the wound deepen and get infected.
How We Prove a Bedsore Contributed to a Nursing Home Resident’s Death
The evidence we use to show the resident died from bedsore complications and not simply with a bed sore includes:
- Wound records, including skin assessments, staging notes, turning documentation, wound-care entries, and photographs to track how severe the bedsore became and whether it was worsening before the resident’s final decline.
- Infection records, any sepsis diagnosis, and the hospitalization timeline make a sequence that can help establish that the bedsore was part of the fatal chain.
- Cultures, lab results, discharge summaries, and transfer records to see whether the infection spread from the wound into the bloodstream or other systems.
- The death certificate, if it lists sepsis or another immediate cause of death, even without clearly tracing that event back to the infected wound.
- Expert testimony to explain whether the resident’s death was medically linked to the bedsore, whether the infection likely began there, and whether the fatal decline would have been less likely if the wound had been prevented or treated properly.
What Types of Compensation Can Families Recover After Losing a Loved One Due to Pressure Injuries?
Families may be eligible to recover the following types of compensation:
- Medical expenses – Covering treatment, hospitalization, and long-term care.
- Pain and suffering – Compensation for the resident’s physical and emotional distress.
- Punitive damages – If the facility’s negligence was particularly reckless.
- Wrongful death – If the neglect led to a fatal outcome, surviving family members may file a claim.
Consult an Experienced Nursing Home Abuse Lawyer!
At the Nursing Home Law Center, we have represented many nursing home residents who have suffered from pressure ulcers and sores. Our nursing home abuse lawyers will investigate your case, protect your rights, assess damages, gather compelling evidence, and even represent you in court if necessary.
The sooner you seek legal advice regarding the bedsore, the sooner we can take action that could potentially save a life. We will also help you seek justice if you have already suffered due to the injury.
Call the Nursing Home Law Center today at 800-926-7565 or complete the online form to request a free consultation.
FAQs
What Is the Average Payout for Fatal Bedsore Cases?
According to Law.com‘s VerdictSearch, payouts in fatal nursing home bedsore cases range from $55,169 to $114,000,000. The average payout is $5,800,570, while the median recovery is $1,208,740.
Several factors can influence the value of a claim, including:
- Stage and severity of the pressure ulcer
- Evidence of neglect
- Duration of suffering
- Causation
- Facility records
- Resident’s overall health
- Regulatory violations
How long do families have to take legal action following a fatal bedsore?
The timeframe to file a nursing home abuse claim varies by state, typically ranging from one to three years from the date of injury or discovery. Missing this deadline could mean losing the right to seek compensation, so acting quickly is crucial.