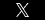Search
Bedsores. Completely Preventable? Absolutely.
Today I met with a family who’s mother recently died from sepsis after a month stay at a Chicago-area hospital. The family hesitantly confided in me that their mother had a gaping hole on her buttocks at the time of her death. While the family obviously was not responsible for their mother’s care when she was in the hospital; they had a sense of responsibility because there is a stigma about bedsores.
 Once you see how gruesome an advanced stage bedsore can be, you will never forget it. Decubitus ulcers, commonly known as bed sores, may start in a small area and look similar to a bruise. If left untreated or gone unnoticed, the bed sores may rapidly develop into literally deep holes in the body. Bedsores are generally categorized I, II, III and IV. A stage IV bedsore may involve dead skin, a putrid smell, and a tunneling which often times results in internal organs becoming visible.
Once you see how gruesome an advanced stage bedsore can be, you will never forget it. Decubitus ulcers, commonly known as bed sores, may start in a small area and look similar to a bruise. If left untreated or gone unnoticed, the bed sores may rapidly develop into literally deep holes in the body. Bedsores are generally categorized I, II, III and IV. A stage IV bedsore may involve dead skin, a putrid smell, and a tunneling which often times results in internal organs becoming visible.
Stages of pressure sores
To some, bedsores are associated with the poor and unwanted. In reality, they are commonplace at many hospitals and skilled nursing facilities. Wherever they develop it is unfortunate and completely preventable. Upon admission, each facility should do an assessment to determine the potential for each resident / patient to develop bedsores. The failure to do a five minute bedsore assessment at many facilities only leads to bigger problems developing more quickly.
I came across this New York Times article discussing the team-approach required to address the prevention of bedsores. Clearly, every person responsible for a resident’s care must keep in mind of the real possibility that bedsores may develop if one member of the team drops the ball.
For more information on nursing homes in Chicago look here. For laws related to Illinois nursing homes, look here.
 Nursing Home Law News
Nursing Home Law News