legal resources necessary to hold negligent facilities accountable.
North Las Vegas Nursing Home Abuse & Neglect Attorneys
 The aging population throughout Nevada has placed a heavy demand on the nursing facilities as more senior citizens require a high level of skilled nursing care. When family members choose to place a loved one in a nursing facility, they expected the nursing home will provide a secure and safe environment. Yet, the North Las Vegas nursing home abuse & neglect attorneys at Nursing Home Law Center LLC have handled many cases of Nevadan nursing home residents who have been abuse, neglect or mistreated that resulted in physical injury, serious harm or death.
The aging population throughout Nevada has placed a heavy demand on the nursing facilities as more senior citizens require a high level of skilled nursing care. When family members choose to place a loved one in a nursing facility, they expected the nursing home will provide a secure and safe environment. Yet, the North Las Vegas nursing home abuse & neglect attorneys at Nursing Home Law Center LLC have handled many cases of Nevadan nursing home residents who have been abuse, neglect or mistreated that resulted in physical injury, serious harm or death.
Medicare releases information monthly to the public on all nursing facilities in North Las Vegas based on inspections, surveys and investigations. Recently, inspectors identified serious deficiencies and violations at fourteen (40%) of the thirty-five North Las Vegas nursing homes that resulted in substandard care that led to avoidable injury and preventable death. Did your loved one suffer harm through mistreatment, neglect or abuse while living in a nursing facility in Nevada? If so, let our team of dedicated lawyers protect your rights starting today. We urge you to contact the North Las Vegas nursing home abuse & neglect lawyers at Nursing Home Law Center (800-926-7565) to schedule a free case evaluation. Let us explain your legal options for filing in resolving a claim for compensation.
Cases involving abuse and neglect against the elderly occurs significantly more frequently than families imagine. The elderly are society’s most vulnerable citizens who are living at the most defenseless point of their lives. Often times their living situation provides no other option than to move into a nursing facility to ensure they receive all the necessary care, medication, and assistance to improve or maintain their quality of life. Unfortunately, nursing home abuse takes on many ugly forms where the elder is taken advantage of in situations that often go unnoticed or undetected.
The cases involving nursing home abuse and neglect is expected to rise in the years ahead. This is because the population of seniors 65 years and older is becoming one of the largest demographics of all groups. Even in North Las Vegas, out of the population of more than 200,000 residents, at least 26,000 are in their retirement years.
North Las Vegas Nursing Home Resident Health Concerns
Our Nevada elder abuse attorneys recognize there are many families who suspect their loved one is being injured, abused or neglected. Our lawyers have long served as nursing home resident advocates. Our extensive knowledge of procedural law, providing evidence and navigating the legal process has assisted families with loved ones harmed by the nursing home industry.
In an effort to provide assistance, our law offices continuously review, evaluate and assess national and state government agency publicly available databases including Medicare.gov. The information we harvest from these databases includes opened investigations, filed complaints, safety concerns and health violations found in nursing facilities all throughout Nevada. Families often use the information we post as an effective tool for locating the best facility in their community to place their aging spouse, parent or grandparent, who requires the highest level of hygiene and health care.
Comparing North Las Vegas Area Nursing Facilities
The list below details nursing facilities all throughout the North Las Vegas area currently maintaining an average and below average rating compared with other facilities all throughout the United States. In addition, our network of attorneys has posted our primary concerns showing evidence of actual cases investigated and reviewed by state surveyors and inspectors at these nursing facilities. Some cases involve an uncontrolled spread of infection throughout the facility, unsanitary conditions, medication errors and a lack of quality care provided to one or more residents.
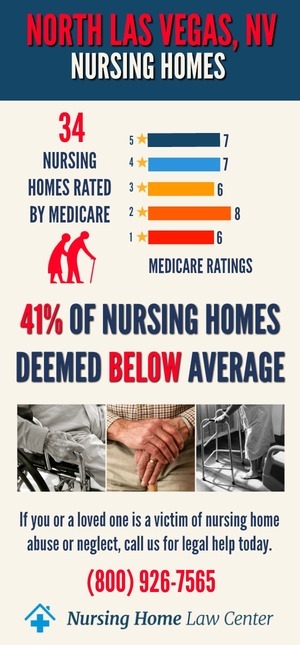
Overall Rating of 35 Nursing Homes
Rating: 5 out of 5 (7) Much above average
Rating: 4 out of 5 (7) Above average
Rating: 3 out of 5 (7) Average
Rating: 2 out of 5 (11) Below average
Rating: 1 out of 5 (3) Much below average
August 2018
NORTH LAS VEGAS CARE CENTER
3215 E. Cheyenne Ave.
North Las Vegas, Nevada 89030
(702) 649-7800
A “For-Profit” 182-certified bed Medicaid/Medicare-participating facility
Overall Rating – 1 out of 5 possible stars

Primary Concerns –
Failure to Provide Residents an Environment Free of Medication Errors
In a summary statement of deficiencies dated 05/15/2015, a notation was made during an annual licensure and certification survey by a state investigator concerning the facility’s failure to “clarify a duplicate order for pain medication” that affected one resident at the facility and a failure “to obtain pain medications in a timely manner” that affected a resident at North Las Vegas Care Center.
The deficient practice was noted by the state investigator conducting a survey at the facility after reviewing a resident’s clinical record that revealed “transfers orders dated 12/20/2015 from acute care facility that included Norco (hydrocodone/acetaminophen)” prescribed at “7 milligrams/325 milligrams every six hours as needed for pain.” However, the surveyor noted an admission order dated 12/29/2015 documenting “an error entry for Norco 7.5 milligrams/325 milligrams every six hours.”
There was an entry indicating the nurse should “see the following page. On that page, the notation “Admission Order documented Norco 5/325 milligrams one tablet by mouth every six hours.
The state investigator noted that the resident’s “clinical record lacked documented evidence a new order for Norco 5/325 milligram every six hours scheduled was obtained on February 2015.
An interview was conducted by the state surveyor 11:40 AM on 05/14/2015 with the facility’s Director of Nursing who “confirmed it was a duplicate order for Norco, one order for Norco as needed and the other for Norco as a scheduled medication.” The facility’s Director of Nursing “indicated pain medication such as Norco were usually ordered as needed […and acknowledged that] the order should be clarified with the [the resident’s] physician.”
The surveyor also noted that the resident’s April 2015 MAR (Medication Administration Record) “revealed 16 doses of Norco are not administered from 03/13/2015 to 03/17/2015.
Our North Las Vegas nursing home neglect attorneys recognize a failing to follow physician’s orders when administering medication could place the health and well-being of the resident immediate jeopardy. The deficient practice by the nursing staff at North Las Vegas Care Center could be considered mistreatment or negligence.
MARQUIS CARE AT CENTENNIAL HILLS
6351 N Fort Apache Rd
Las Vegas, Nevada 89149
(702) 515-3000
A “For-Profit” 120-certified bed Medicaid/Medicare-participating facility
Overall Rating – 3 out of 5 possible stars

Primary Concerns –
Failure to Follow Procedures and Protocols for a Resident Who Was Full Code and Later Expired after a Delay in Transferring the Resident to an Acute Facility
In a summary statement of deficiencies dated 07/16/2015, a complaint investigation was opened against the facility for its failure to “transfer resident in a timely manner.” The investigation is in response to an order set indicating the resident “was a full code. Code status: CPR (Cardiopulmonary Resuscitation) and call 911 was listed in the order set.”
The investigation included a review of the facility’s Progress Notes in the medical record that documented: “a day shift nurse documented the resident refused to have supplement and for different medications at 11:31 AM.”
By 2:23 PM “the last set of documented vital signs were entered in the medical record: blood pressure, oxygen saturation 88%; pulse 120; temperature 98.8 Fahrenheit.” The nurse on duty documented “the resident was unable to swallow three different medications at 4:56 PM (so, the medication was held).” One minute later, the nurse documented “shortness of breath and apnea and administered an opiate pain medication.” By 5:06 PM, the nurse documented “unable to obtain residents oxygen saturation level.”
The state surveyor conducting the investigation into the filed complaint noted that “the medical record lacked documented evidence a nurse assessed the resident for a Change of Condition or obtained vital signs (blood temperature, pulse rate, respiration rate (rate of breathing) and blood pressure.” In addition, the medical record also “lacks documented evidence a nurse notified a physician.”
The Nurse’s Notes also revealed that a nurse indicated Full Code residents were transferred out of the facility. When asked why vital signs were not obtained, [the nurse] indicated vital signs were not requested by the Nurse in Charge during the shift […and] indicated vital signs should be obtained within an hour or less of a transfer.”
At some point “prior to 7:35 PM, clarified by [a nurse on duty] at 4:00 PM, the nurse notified hospice the resident needed to be transferred […and] expected hospice to notify the physician. The medical record lacked documented evidence the physician notification occurred. The hospice nurse told [the nurse on record] to follow the Skilled Nursing Facility’s protocol.
By 9:00 PM, the nurse “documented the resident was unresponsive with frequent episodes of apnea, cold/clammy/pale skin and unable to obtain oxygen saturation.” In addition, there were still no documented evidence of a change in the resident’s condition and also that “the medical record lacked documented evidence a nurse notified a physician.” At 11:00 PM, “the facility transferred the resident to acute care.”
An interview with the attending nurse revealed that “the facility transferred full code residents out with a change in condition […and] told the nursing assistant to obtain a resident’s vital signs, but the nursing assistant did not enter them.” That nurse was also “asked to identify the nursing assistant, was unable to do so. The vital signs documented 2:23 PM [that they] were the same as the Facility Transfer Form at 11:00 PM [on the night of the resident was transferred].”
It was also revealed that on the afternoon of the incident the nurse “indicated the non-emergency number for emergency medical services was called instead of 911.” When asked to distinguish an emergency versus nonemergency transfer, the nurse indicated “an emergency would be if vital signs were abnormal for an unexplained reason, like an oxygen saturation less than 80%.” However, it was noted that “the first oxygen saturation recorded at the acute care facility at approximately 1:54 PM the night of the transfer was 80% with the resident receiving 15 liters of oxygen. The resident was intubated and put on a ventilator […and] received liters via nasal cannula at the facility.”
The state investigator asked the nurse “why 911 was not utilized.” However, the nurse “did not know but indicated 911 should have been called instead of the non-emergent number. When asked why the family was call before activating emergency medical services, [the nurse] indicated feeling pressured.”
An interview was conducted by the state investigator with the facility’s Director of Nursing who “indicated in the given scenario of the resident in question, it was an emergency when nurses could not obtain the resident’s oxygen saturation, and when the resident was unresponsive. Vital signs should have been taken, 911 should have been called, alert charting with a full assessment should have been completed. Despite documented changes occurring several hours prior during the shift, [the nurse] did not transfer the resident until 11:00 PM.” Notations in the medical records indicate “the resident later expired.”
Our Las Vegas elder abuse lawyers recognize a failing to follow protocols when a resident is in full code and their order set indicates transfer the resident in a timely manner could place the health and well-being of the resident in immediate jeopardy. The deficient practice by the nursing staff at Marquis Care at Centennial Hills might be considered negligence or mistreatment, especially because the delay in transferring the resident to an acute facility might have led to their death. The actions by the nursing staff did not follow the facility’s policy titled: Change in a Resident’s Condition or Status that reads in part:
“Charge nurse will notify the resident’s attending physician or on-call physician when there has been a reaction to medication, significant change in the resident’s condition, or refusal of treatment or medications two or more consecutive times.”
The resident will be assessed by the Licensed Nurse on Duty. The assessment shall include as appropriate, but not limited to vital signs, loss of consciousness, onset, duration and severity of the change.”
The licensed nurse will notify the physician and the responsible party and document in the clinical record the date, time of notification the person informed.”
“Should it become necessary to make an emergency transfer or discharge to a hospital or other related institution, our facility will implement the following procedures: call 911; notify the resident’s attending physician.”
GAYE HAVEN INTERMEDIATE CARE FACILITY
1813 Betty Lane
Las Vegas, Nevada 89156
(702) 452-8399
A “For-Profit” 20-certified bed Medicaid/Medicare-participating facility
Overall Rating – 1 out of 5 possible stars

Primary Concerns –
Failure to Follow Physician’s Orders to Ensure Necessary Care Is Provided and an Alteration Is Required in Their Prescribed Treatment
In a summary statement of deficiencies dated 07/23/2015, a state surveyor made a notation during an annual licensure and certification survey concerning the facility’s failure to “ensure necessary care was provided in accordance with the resident’s physician’s orders and their Plan of Care” that affected one resident at the facility. In addition, the facility also “failed to ensure [residents were] notified when a need to alter the prescribed treatment occurred.” This failure affected three residents at Gaye Haven Intermediate Care Facility.
A state investigator reviewed a resident’s Care Plan documenting that “the resident was at risk for pressure ulcers due to the resident not remembering to reposition in bed. Certified Nursing Assistants (CNAs) were to perform skin checks to monitor for skin breakdown.”
The deficient practice was noted after a 10:22 AM 07/22/2015 interview with a facility’s CNA who “located in a notebook where the daily skin checks would belong. The notebook lacked documented evidence the skin checks for the resident were documented. The CNA confirmed the skin checks were not documented.”
In addition, the state investigator reviewed the resident’s physician’s orders and MAR (Medication Administration Record) revealing medication prescribed by the resident’s doctor “was not given on 07/06/2015” to treat hypertension and blood pressure. Documentation of the resident’s MAR (Medication Administration Record) “revealed a BP (blood pressure) of 98/58. The record lacked documented evidence the medication was held for the low blood pressure [as prescribed by the resident’s physician]. In addition, the resident’s records lacked documented evidence the blood pressure was rechecked within an hour or that the physician was notified.”
The MAR revealed that on 07/16/2015, the medication was not administered to the resident even though the documentation reveals the resident had a blood pressure of 100/68 the resident’s 102/86 blood pressure. However, the records “lacked documented evidence the blood pressure was rechecked within an hour or that the physician was notified.
The state surveyor noted that the medication according to the resident’s MAR (Medication Administration Record) was not administered to the resident between 07/01/2015 and 07/07/2015. However, there was documentation indicating that “the medication was refused by the resident between 07/02/2015 and 07/05/2015. Even so, the resident’s records lacked the “documented evidence the physician was notified [that] the medication was discontinued on 07/07/2015.”
An interview was conducted by the state investigator at 1:45 AM on 07/23/2015 with the facility’s Director of Nurses who “indicated the resident’s blood pressure should be documented on the MARs, including the repeat blood pressures.” The Director of Nursing also explained that “any medications that are refused should prompt a call to the physician to report a refusal, and the call to the physician should be documented in the Nurse’s Notes.”
Our Las Vegas nursing home neglect attorneys recognize that failing to follow procedures and protocols when administering medications as per a physician’s orders could have life-threatening consequences to the resident. The deficient practice by the nursing staff in failing to notify the resident’s physician might be considered mistreatment or negligence. In addition, the action by the nursing staff did not follow the facility’s revised February 2014 policy titled: Change in a Resident’s Condition of Status reads in part:
“The Nurse Supervisor/Charge Nurse will notify the resident’s Attending Physician or On-Call Physician when there has been: A need to alter the resident’s medical treatment significantly. [In addition], the Nurse Supervisor/Charge Nurse will record in the resident’s medical record information relative to changes in the resident’s medical/mental condition or status.”
Abuse and Neglect Are Widespread Nursing Home Problems
The level of abuse and neglect occurring in nursing facilities has become epidemic. The widespread problem often results in severe harm, preventable injury or the death of the resident. The most common types of abuse that occur in nursing facilities involve:
- Physical Abuse including kicking, slapping, hitting, pushing, or the unnecessary/unauthorized use of physical restraint.
- Sexual Assault including any unwanted/nonconsensual sexual conduct
- Negligence including a failure to provide a proper level of care that could result in facility acquired bedsores, malnutrition, dehydration or injuries caused by falling
- Drug Abuse including under medicating or overmedicating residents
- Mental Abuse often caused by derogatory or degrading comments, offensive language or constant criticism
- Emotional Trauma caused by isolating the resident from other residents, visitors, family, friends or caregivers
- Financial Exploitation where residents, visitors, family members or caregivers steal the resident’s money, goods or property
Indicators of abuse often encompass various significant changes in the resident’s behavior including anger or withdrawal, unexplained bruises and broken bones, frequent cuts or lacerations, deteriorating physical appearance or signs of fear and intimidation.
If you suspect your loved one has become a victim of abuse or neglect, it is imperative to take immediate action by contacting a personal injury attorney who specializes in nursing home abuse cases.
Hiring a Lawyer
We encourage you to contact the North Las Vegas nursing home abuse attorneys at Nursing Home Law Center LLC to discuss all aspects of the situation, event or your concerns. Our team of dedicated Nevada elder abuse attorneys will focus our attention on the information you provide and offer various legal remedies to end the harmful or abusive acts against your loved one. In addition, we will provide comprehensive details on how the legal process in Nevada works and the efforts we can take to pursue the financial recompense you and your loved one deserves.
We encourage you to make contact with our Clark County elder abuse law office today by calling (800) 926-7565 to schedule your no obligation, free full case review. We will take steps to immediately gather documentation and evidence to support your claim and handle all aspects of your case during the sensitive time. All information you share with our law offices remains confidential to ensure the privacy and protection of your loved one. We accept all nursing home abuse cases, personal injury claims and wrongful death lawsuits through contingency fee arrangements. This means no upfront fees are required to receive immediate legal representation.
For additional information on Nevada laws and information on nursing homes look here.
Nursing Home Abuse & Neglect Resources
If you are looking for information on a specific facility or an attorney, please see links below to respective locality pages.
- Carson City
- Elko
- Enterprise
- Henderson
- Las Vegas
- North Las Vegas
- Paradise
- Reno
- Sparks
- Spring Valley
- Sunrise Manor
 Clark County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
Clark County Nursing Home Injury Attorney Nursing Home Law Center LLC Home