legal resources necessary to hold negligent facilities accountable.
Oklahoma Nursing Home Abuse Lawyers
Contact our nursing home abuse lawyers today if your loved one was harmed by negligent or abusive staff members.
Schedule a free consultation to discuss the merits of filing a compensation case.
The United States Congress enacted federal laws to ensure that nursing home residents are treated with the dignity, respect, and care they deserve.
The 1987 Nursing Home Reform Act protects residents rights, including the right to:
- Be informed of changes in their medical treatment
- Be treated with dignity and respect
- Be free from abuse and neglect
- Be free from physical or chemical restraints
- Receive confidentiality in the maintenance of patient records
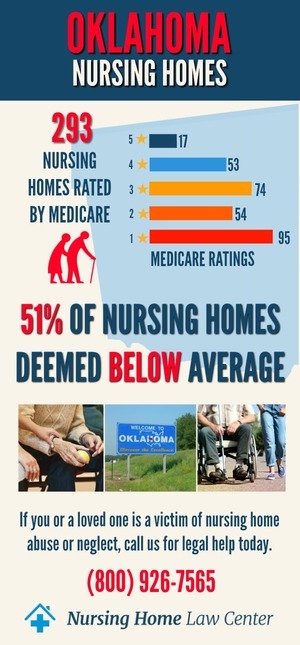
According to Medicare-collected data, there are currently 304 nursing homes rated in Oklahoma monitored by the federal agency through inspections, investigations, and surveys.
Of these, 104 (thirty-four percent) Oklahoma nursing facilities are rated below the national average because investigators found severe violations and deficiencies that led to resident harm and wrongful death.

Nursing Home Care Must Be Thorough
The elderly and disabled often resist moving into a nursing facility because historically, society looks at an "old folks' home" as a place to go die. However, the care provided in a long-term care facility might be precisely what someone you love needs to survive.
The nursing staff will continuously monitor the patient's health, administer medications according to doctor's orders, and assist with meals and personal hygiene.
A caregivers' home is a challenging environment requiring residents to give up their privacy in exchange for continuous care.
Signs of Abuse in Nursing Homes
According to the National Center on Elder Abuse, the common signs associated with elderly abuse include:
- Physical assault involving cuts, bruises, lacerations, broken bones,
- Sexual assault including unexplained sexually transmitted diseases, and rape, sodomy, inappropriate touching, unexpected vaginal or anus bleeding, and sexual coercion
- Financial exploitation where caregivers, families, visitors, and other residents gain illegal access to the victim's cash, credit cards, bank accounts, and belongings
- Negligence where the victim suffers from unexpected weight loss, medication errors, malnourishment, dehydration, poor hygiene, social isolation, and pressure wounds (bed sores)

A Nursing Home Is Legally Responsible for Your Loved One
Nearly every state's legislative body has enacted filial support laws requiring a parent's adult children to provide financial support if they can not care for themselves.
An adult child will likely need to pay their parents' medical bills, including the cost of assisted-living facilities.
The child must ensure that the parent receives sufficient shelter, clothing, food, and medical/health care.
That said, Oklahoma does not currently have a finial support law holding children legally responsible for providing their parents necessities when they cannot do so without assistance.
Can an Elderly Person Refuse to Go to an Oklahoma City Nursing Home?
While many families want someone they love to receive the best care in a safe environment, it might be challenging to convince a reluctant parent or spouse to relocate.
Many individuals will outrightly refuse to go even if it is in their own best interests to support their health and well-being.
Tension among family members could rise quickly if the parent or spouse has Alzheimer's disease or dementia and resists relocating. Some spouses and adult children use "compassionate deception" to convince someone you love to try the facility out for a limited time, like a week or a month, to "see" if they like.
Who Is at Risk for Nursing Home Abuse?
According to the CDC (Centers for Disease Control and Prevention), nearly two million American adults are abused and mistreated every year at home and in nursing care facilities.
Those most at risk of mistreatment include:
- People with mental illnesses
- Cognitively impaired residents with Alzheimer's disease or dementia
- Patients with inadequate coping skills
- People with previous abuse exposure usually in childhood
- Nursing facility residents with extremely aggressive behavior
- Residents in nursing facilities with chronic staffing problems
- Assisted living home residents subjected to staff burn out, administrative oversight, and stressful working conditions
Adult children and spouses could take steps to reduce the chances of a loved one being mistreated in a nursing facility by routinely visiting them in their room or common areas.
Families should also ensure that the facility has effective monitoring systems, provides routine employee training, and staff follows established institutional procedures and policies on patient care.
Common Examples of Nursing Home Neglect and Elder Abuse
According to the National Center on Elder Abuse, typical examples of neglect and abuse in nursing facilities could include:
- Physical abuse
- Sexual abuse
- Mistreatment
- Malnutrition
- Unexplained weight loss
- Psychological abuse
- Psychosocial isolation
- Financial exploitation
- Avoidable falls
- Medication errors
- Failing to follow physician's orders
- Physical and chemical restraints
Filing a Complaint on Behalf of Elder Abuse Victims
Do you suspect that an individual is being abused or neglected in an assisted living facility? Any suspected mistreatment should be reported to appropriate authorities in Oklahoma.
Filing a report of nursing home neglect or abuse is vital to protect the victim. All too often, residents suffer additional harm if others fail to file a report.
Nursing home workers might believe that they will not be caught abusing or neglecting a resident, so they continue to engage in these heinous acts until a report is finally filed.

Know Your Loved One's Many Legal Rights in a Nursing Home Abuse Case
Understanding your loved one's legal rights in a nursing facility allows you to act quickly when necessary.
Knowing state and federal revelatory laws ensures that you will not be persuaded that staff members might not be abusing your loved one when they are.
Trust your gut when a loved one complains about harm or shows physical signs of abuse or neglect. Take action to file a report so that you can know everything was done to protect the legal rights of your loved one.
Talk with Oklahoma Nursing Home Negligence Lawyers Today
Attorneys can provide you with OK nursing home information and help you resolve your legal issues. Our injury attorneys are available to investigate any claims of abuse or neglect.
Our legal team has experience in dealing with the nursing facility staff workers and administrators. Your injury lawyer can empower you during this challenging situation.
Our nursing home negligence lawyers are available to help residents throughout the state of Oklahoma in areas such as:
- Broken Arrow
- Edmond
- Enid
- Lawton
- Midwest City
- Moore
- Norman
- Oklahoma City
- Stillwater
- Tulsa
Are you unsure how to proceed in filing a report of abuse, mistreatment, or neglect about an Oklahoma City nursing home?
Speak with a nursing home abuse lawyer in Oklahoma City OK and throughout Oklahoma to learn more.
Frequently Asked Questions About Nursing Home Injury Lawsuits
Here are the answers to some commonly asked questions that people ask of a nursing home abuse attorney:
What Types of Nursing Home Abuse Can I Sue For?
A nursing home resident may experience a number of different types of abuse. Your loved one may encounter:
- Physical abuse
- Sexual abuse
- Bed sores
- Financial exploitation
- Emotional abuse
You should contact adult protective services if your loved one is a victim of nursing home abuse.
This does not diminish your ability to file a lawsuit. Experienced nursing home abuse attorneys can evaluate your situation and advise you of your legal rights and options. Contact our team today for a free consultation.
What Else Would Allow Me to File a Nursing Home Lawsuit?
Nursing home neglect is a common reason for a lawsuit. Instances of neglect include:
- Failure to obtain medical care as necessary
- Nursing home employees allowing your loved one to contract an infection by not taking care of their hygiene
- Dehydration and malnutrition
Call us if your family member has been injured by the failure to provide the appropriate care during an admission to a nursing home.
How Much Can an Attorney Help Me Recover?
This all depends on the harm that your loved one has suffered and the actions of the nursing home staff. Each nursing home abuse claim is valued differently.
Some factors in the overall award would include:
- Your loved one's age
- The amount that they suffered
- The level of culpability on the part of the nursing home
- Any aggravating factors that could lead to punitive damages

Personal Injury Lawyers Acting on Behalf of Your Family Member
The Oklahoma City nursing home abuse attorneys at the Nursing Home Law Center can help families with loved ones who were abused or neglected.
Our law firm will help you file a lawsuit against the care facility where your family member was injured.
If you see signs of nursing home abuse, call our phone number today at (800) 726-9565 today for a free consultation.
Once we begin the attorney-client relationship, we can provide you with legal advice about your claim.
Oklahoma State Resources for Victims of Nursing Home of Abuse and Neglect
Here are some places where you can contact for help and emergency assistance:
- Oklahoma Family Support Services Division, Adult Protective Services
- Oklahoma Aging Services Division
- Oklahoma Aging Services Division: Long Term Care Ombudsman
Pressure wounds develop in areas with restricted blood flow caused by the patient's body weight pushing against a pad, chair, or mattress. Restricting blood flow minimizes oxygen delivery to the skin and underlying tissue.
Deprivation of oxygen to the affected area injures the skin's dermis and epidermis layers that could start to die or be permanently damaged.
Our long-term care facility negligence attorneys currently represent individuals and families in lawsuits against facilities where a pressure sore developed or worsened. We handle our nursing home abuse cases on a contingency fee basis where we only charge for our legal fees when there is a financial recovery for you.
Complete the contact form here for a free case review.
Routine Skin Inspections Needed to Identify & Treat Pressure Wounds
 The nursing home staff must provide each patient with premium around-the-clock Health Care and perform routine skin inspections to identify any developing sores. During the initial stage, a pressure ulcer appears as a fluid-filled blister with red dots or an inflamed area that feels cooler or warmer than the surrounding tissue.
The nursing home staff must provide each patient with premium around-the-clock Health Care and perform routine skin inspections to identify any developing sores. During the initial stage, a pressure ulcer appears as a fluid-filled blister with red dots or an inflamed area that feels cooler or warmer than the surrounding tissue.
The nursing staff must alleviate the pressure at the first signs of developing bedsores. Within days, the wound can heal entirely with ongoing care.
However, if the area is left unattended, it can quickly decline to an advanced stage where a small crater develops, exposing fat deposits. Any developing crater could decline to a life-threatening stage causing the area to become susceptible to skin infections (sepsis) or bone infections (osteomyelitis).
At its most critical stage, the crater deepens to expose bone and muscle below. Without effective antibiotics, the patient can quickly die from a compromised immune system.
Performing routine skin inspections could eliminate all advancing stages of developing pressure wounds. Doctors treating decubitus ulcers use various procedures, including debridement where the dead or dying tissue is cut away from the wound.
Most facility-acquired pressure wounds are caused by negligence. With proper treatment, the wound could have easily been prevented or not allowed the opportunity to progress to a crucial stage.
Why Routine Adjustments Are Necessary to Reduce Build Up of Pressure
When caregivers routinely adjust the patient's body every two hours or less, the potential of developing a bedsore is nearly eliminated. Successful nursing homes with a good track record usually follow scheduled turning and readjusting protocols for every mobility-challenged patient.
Unfortunately, many bedridden and individuals who use wheelchairs are unable to reposition themselves without assistance.
Holding the Nursing Home or Hospital Accountable for Skin Sores
Nearly all pressure ulcers are preventable, and any sign of a loved one suffering a bedsore is typically an indicator of negligence by the medical team. Negligence is often the result of improperly trained staff members not following proven protocols to minimize the potential of developing a sore.
Many families with a loved one suffering from a pressure sore are proactive and will hire an Oklahoma nursing home abuse attorney to stop the negligence immediately.
Our Oklahoma negligence law firm can provide family members with numerous legal options to seek financial compensation for damages, report what happened to proper authorities, and hold the nursing home accountable. The lawyers can also send medical personnel into the nursing facility to properly treat the patient's life-threatening condition.
Our team provides legal services in cities throughout the state, including:
- Oklahoma City
- Tulsa
- Norman
- Lawton
- Broken Arrow
Fill out the form here to contact an Oklahoma pressure ulcer attorney from the list below. These law firms accept nursing home negligence cases on contingency and provide legal services to help stop the abuse and assist families seeking financial compensation for damages.
Our attorneys follow social distancing guidelines to prevent the spread of Covid-19 (coronavirus).
Did you notice any signs of nursing home abuse involving your loved one? Take the first step now to open a personal injury case.
Nursing Home Negligence
STATUTE OF LIMITATIONS- 2 years with Discovery Rule. (Okla. Stat. Ann. Title 12, §95)
- Medical malpractice – 2 years with Discovery Rule. An action brought more than three years from the injury date is limited to past and future actual medical and surgical expenses regarding the injury.
In the case of a minor under age twelve, the parent or guardian must bring suit on behalf of the minor within seven years after the malpractice. If the minor was injured at age twelve or older, the plaintiff has until one year after turning eighteen to file suit. (Okla. Stat. Ann. Title 76, §18; Okla. Stat. Ann. Title 12, §96)
DAMAGES CAP- Punitive damages are limited to $100,000; in the case of intentional and malicious acts, punitive damages are limited to the greater of $500,000, or two times, compensatory damages. (Okla. Stat. Ann. Title 23, §9.1)
Wrongful Death
STATUTE OF LIMITATIONS- 2 years from the time of death. (Okla. Stat. Ann. Title 12, §1053)
- None.
State Resources
Nursing Home Care State Law
- Protective Services for Vulnerable Adults Act – (Okla. Stat. Title 43a, §§10-101 – 110)
 Oklahoma Nursing Home Injury Lawyer Nursing Home Law Center LLC Home
Oklahoma Nursing Home Injury Lawyer Nursing Home Law Center LLC Home


