The Nursing Home Law Center is committed to providing the legal resources necessary to hold negligent facilities accountable.
Nursing Home Bedsore Lawyer
Experienced Nursing Home Abuse Attorneys Handling Bedsore Cases
If your loved one has developed bedsores while in a healthcare facility, you may be eligible to recover compensation on their behalf. Contact us now to request a free consultation with a nursing home bedsore lawyer.
What Are Bed Sores?
Bedsores, also called pressure sores or decubitus ulcers, occur when hospitals and nursing homes leave a patient in the same position for prolonged periods, cutting off blood flow and damaging the skin and underlying tissue.
Although entirely preventable with adequate care, bedsores are a persistent issue in nursing homes and often signal neglect or abuse. If the assisted living facility or nursing home your loved one is in has failed to prevent bed sores, you must take action.
What Causes Bed Sores?
Residents with limited mobility or those who are bedridden are at the highest risk of developing these injuries. Prolonged pressure on the shoulder blades, tailbone, and heels restricts circulation, leading to tissue damage, open wounds, and potential infection.
Nursing home staff are responsible for repositioning residents regularly to maintain healthy blood flow and prevent pressure sores. However, failure to meet this standard of care is common, often leading to severe complications. To make matters worse, many insurance companies deny coverage for bedsores caused by staff negligence, creating further obstacles to proper treatment.
Why You Need a Nursing Home Bedsore Attorney
When a loved one suffers from bedsores due to negligence, legal representation is essential. Our experienced bedsore lawyers can investigate the underlying causes, gather evidence, and hold the responsible parties accountable.
By pursuing a claim, families can seek compensation for medical expenses, pain and suffering, and long-term care needs, ensuring that no neglect goes unpunished.
Our legal team has a proven track record of securing significant settlements and verdicts for victims of nursing home neglect, including those suffering from bedsores. Below are some examples of the successful outcomes we have achieved on behalf of our clients.
Bedsore Settlements We’ve Won for Injured Nursing Home Residents
- $3,800,000 settlement for a patient who developed a stage 4 bed sore during a short-term rehab stay. Staff failed to regularly reposition the resident, leading to advanced wounds and death from sepsis.
- $1,125,000 settlement after a resident developed multiple untreated bed sores, causing severe infections that led to fatal complications.
- $765,000 settlement for a family after a nursing home resident’s bed sores worsened to a life-threatening condition due to negligent care.
- $920,000 settlement for a resident who developed severe bed sores on their heels. The facility’s failure to follow a care plan resulted in infections requiring debridement surgeries.
- $2,333,333 settlement for an elderly man who developed bed sores on his coccyx. Despite explicit medical orders for repositioning, staff negligence allowed the sore to worsen, leading to his death.

How Bedsore Stages Affect Lawsuits?
Bedsores progress through four stages, each representing increasing severity. These stages are critical in determining the strength and potential value of a bed sore lawsuit, as advanced stages often indicate prolonged neglect or nursing home abuse.
A pressure injury lawyer can help families understand the legal implications of each stage and seek justice for the harm caused.
Stage 1
This is the mildest form of a pressure ulcer, in which the skin appears red or discolored but remains intact. If treated promptly, a bedsore at this stage can heal quickly with no long-term damage. However, even a Stage 1 pressure sorecan indicate inadequate care.
Stage 2
The skin begins to break open in this stage, forming a shallow wound. This stage may cause pain and expose the deeper layers of skin. Stage 2 bedsores are more concerning and suggest that proper preventive measures, such as repositioning and monitoring, have not been followed.
Stage 3
The pressure injuries have progressed deeper, affecting the fatty tissue beneath the skin. The pressure ulcer resembles a crater and increases the risk of infection. Stage 3 bed sores are often indicative of severe neglect and significantly increase the risk of long-term harm to the patient.
Stage 4
This is the most severe stage, where the sore extends to the muscle and bone. Infection is common, and complications such as sepsis or death may result. Stage 4 bed sores are a clear indicator of extreme neglect, and lawsuits involving this stage typically result in higher compensation due to the severe harm caused.
As the severity of bed sores progresses through these stages, the legal case becomes stronger. Advanced-stage bedsores often signal extended neglect and can result in life-threatening conditions, directly impacting the potential compensation a family may receive in a bedsore lawsuit.

What Are the Statistics of Bed Sores in Nursing and Assisted Living Facilities?
Today’s nursing homes and hospitals experience higher rates of pressure sores than in previous decades. Budget cuts, staffing shortages, and undertrained nurses have created an environment where patient care is often inadequate.
Many nurses are overworked and underqualified for their assigned responsibilities, leading to lapses in essential preventive care. Bedsores remain a significant and preventable issue in nursing homes and hospitals.
According to the Centers for Disease Control and Prevention (CDC), over 10% of patients in nursing homes suffer from pressure sores, with approximately half of these cases classified as Stage III or Stage IV, severe wounds involving deep tissue damage and increased risk of infection. Pressure sores are considered a “never event” in healthcare settings, meaning they should never develop under proper care and supervision.
Prevalence and Poor Treatment
As many as 11% of residents in nursing homes have at least one pressure sore, but only 35% of these individuals receive the necessary treatment to promote healing, according to CDC reports. Without adequate care, bedsores can be deadly.
Patients with untreated pressure ulcers are 2 to 6 times more likely to die from complications compared to other severe health conditions, such as cardiovascular disease and cancer. Shockingly, some studies report that pressure sore prevalence in certain nursing facilities can reach as high as 91%, and 60% of patients who develop serious pressure ulcers die within a year of the injury.
Who Is Most At Risk?
The most common victims of pressure ulcers are individuals over the age of 60 with limited mobility, which prevents them from independently moving or repositioning themselves. Bedsores are far more common in nursing homes than in hospitals or in-home elder care.
This is primarily attributed to systemic understaffing within nursing homes, leaving at-risk patients without the necessary attention to prevent or treat skin breakdown. When patients are neglected—especially when left lying in soiled bedding—bedsores can progress rapidly and become infected, leading to serious complications.
Although nursing homes account for the majority of pressure injury cases, hospital-acquired bedsores are also common and are often attributed to patient neglect. According to the National Library of Medicine, patients admitted to hospitals from nursing homes are more than five times more likely to present with pressure ulcers compared to other patients.
What Is the Main Cause of Bed Sores?
The leading cause of pressure ulcers is staff failure to turn and reposition patients regularly, which is necessary to maintain healthy blood flow to the skin. Secondary causes include dehydration and malnutrition, both of which weaken the skin and increase the likelihood of breakdown.
What Is the Cost of Treating Bed Sores?
Treating bedsores can be financially burdensome, with the average cost of care reaching $127,185 according to one study. For many facilities, this expense disincentivizes proper treatment, leaving residents at risk of worsened injuries.
Filing a lawsuit not only helps families secure compensation for medical costs, pain, and suffering but also pressures negligent facilities to improve their standards of care, ultimately protecting future residents from similar harm.
What Are Common Causes of Pressure Ulcers in Nursing Homes?
Several factors can lead to the development of pressure sores in nursing home or hospital patients, with most cases linked to neglect or improper care:
- Immobility: Residents who are bedridden or wheelchair-bound are at the highest risk of developing a bed sore. Prolonged immobility restricts blood flow to certain areas of the body, causing tissue damage. Without frequent repositioning, these nursing home patients are highly susceptible to bedsores.
- Poor Nutrition: Residents who are malnourished or dehydrated are more vulnerable to developing pressure ulcers. Proper nutrition and hydration are essential for maintaining healthy skin and promoting wound healing.Failure to provide adequate food is a sign of neglect in many cases of bed sore development.
- Inadequate Staffing: Many nursing homes suffer from understaffing or a lack of adequately trained staff, making it challenging to provide each resident with the necessary care. When nursing homes are inadequately staffed, patients may not receive the repositioning, hygiene, or monitoring needed for bedsore prevention.
- Failure to Reposition Patients: One of the most important preventive measures for avoiding a bed sore is regularly changing the position of immobile residents. Nursing homes that fail to implement these practices increase the risk of pressure ulcer development, often due to staff neglect and medical malpractice.
What Are the Dangers of Untreated Bed Sores?
If left untreated, a bed sore can lead to a range of severe and life-threatening complications. The progression of a pressure ulcer can result in:
- Infections: Open wounds from bed sores can quickly become infected. If the infection spreads, it can lead to more severe conditions, such as cellulitis or even bloodstream infections.
- Sepsis: One of the most dangerous complications of an untreated bed sore is sepsis, a life-threatening response to infection. Sepsis can cause organ failure and lead to death, making early intervention critical.
- Osteomyelitis occurs when an infection spreads to the bones, causing severe damage and requiring extensive medical treatment.
- Death: In extreme cases, an untreated bed sore, particularly at Stage 4, can lead to wrongful death. The combination of infection, sepsis, and organ failure poses a significant threat to the lives of residents.

What Goes Into Bedsore Prevention in Nursing Homes?
Nursing homes are expected to implement various preventive measures to reduce the risk of developing pressure injuries among residents. Some of the critical steps that should be taken include:
- Regular Repositioning: Bedridden patients must be repositioned regularly to relieve pressure on vulnerable areas such as the shoulders, back, and hips. This is one of the most effective ways to prevent a bed sore from forming.
- Proper Nutrition and Hydration: Ensuring residents receive a balanced diet with adequate hydration is crucial for maintaining skin integrity and preventing bed sores. Nursing homes are responsible for monitoring their residents’ nutritional status and providing necessary supplements if necessary.
- Hygiene and Skin Care: Keeping residents clean and dry helps prevent skin breakdown. Nursing homes must ensure that residents receive regular bathing, incontinence care, and proper wound care when necessary.
- Use of Special Equipment: Pressure-relieving devices such as specialized mattresses or cushions can help reduce the risk of pressure ulcers in residents who are immobile for long periods.
- Staff Training: Nursing home staff must be trained in pressure ulcer prevention, early detection, and wound care. Proper education and protocols can prevent pressure ulcers from developing or worsening.
What Are Nursing Homes’ Legal Duties?
Nursing homes are legally obligated to provide a certain standard of care to their residents, including taking steps to prevent the development of bedsores. Federal and state regulations set clear expectations for how nursing homes must care for their patients.
Under the Nursing Home Reform Act, facilities must ensure that residents receive proper treatment and services to prevent pressure ulcers and other preventable injuries.
Failing to meet these obligations constitutes negligence when nursing homes do not provide adequate care—whether due to understaffing, lack of training, or poor management—they can be held legally responsible for any harm to residents.
If a loved one has developed bedsores while in a nursing home, families have the right to file a nursing home abuse claim, seeking compensation for the harm caused by the facility’s negligence.

Who Is Eligible to File a Bed Sore Lawsuit?
Understanding who is eligible to file a nursing home bedsore lawsuit is essential in taking the necessary steps toward justice.
- Nursing Home or Hospital Residents: The primary person eligible to file bed sore lawsuits in a nursing home pressure sore case is the resident who suffered harm from pressure ulcers. If a resident develops a serious pressure ulcer because of neglect in a nursing home, they have the legal right to file a claim against the facility.
- Family Members: In many cases, family members, such as spouses, adult children, or siblings, can file a lawsuit on behalf of their loved one. If the resident is still alive but unable to take legal action, the family may step in to seek compensation for the harm caused by the nursing home. In cases where a resident has died from complications related to bedsores, family members may pursue a wrongful death lawsuit.
- Legal Guardians: If the resident has been declared legally incapacitated, a legal guardian may be appointed to make decisions on their behalf, including filing lawsuits for nursing home neglect or elder abuse. The guardian assumes responsibility for protecting the resident’s legal rights.
- Power of Attorney Holders: If the resident granted power of attorney to a family member or another individual before becoming incapacitated, that person can file a lawsuit on behalf of the resident. The power of attorney gives them the legal authority to make decisions, including taking legal action against a nursing home for neglect and elder abuse.
Why Choose Nursing Home Law Center
At Nursing Home Law Center, we are dedicated to protecting the rights of elder care facility residents who have suffered from abuse and neglect, including the development of painful and preventable bedsores.
Our team of experienced nursing home pressure ulcer attorneys has successfully handled numerous pressure ulcer cases, holding negligent facilities accountable for the harm they cause.
We understand the physical, emotional, and financial toll that bedsores take on victims and their families. With our compassionate client service, we work closely with families to seek justice and secure the compensation they deserve.
Our expertise allows us to navigate the complexities of these claims and fight aggressively for the best possible outcomes.
Filing a Nursing Home Bedsore Lawsuit
When a resident develops bedsores due to neglect, families have the right to seek legal recourse through a bedsore lawsuit.
Filing a lawsuit can help hold assisted living facilities or nursing homes accountable and secure financial compensation for medical expenses, pain and suffering, and other related damages. However, filing a successful nursing home bedsore lawsuit requires careful planning and a clear understanding of the necessary legal steps.
What Evidence Is Needed for a Successful Lawsuit?
For a bedsore lawsuit to be successful, gathering strong evidence is essential. Some of the most critical pieces of evidence include:
- Medical Records: Detailed medical documentation showing the resident’s condition, the development and progression of bedsores, and the nursing home’s treatment (or lack thereof). These records are vital in proving negligence and substandard care.
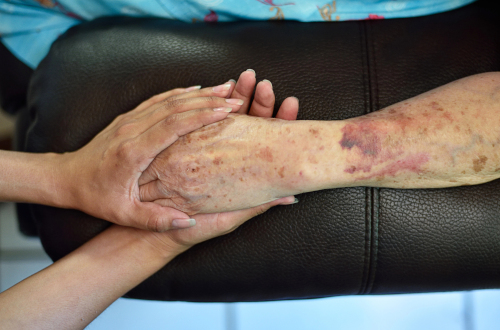
- Photographs: Photographs of the affected area at different stages can visually demonstrate the severity of the pressure ulcers. These images show how the bedsores developed and whether they worsened due to a lack of care.
- Witness Statements: Statements from family members, other residents, or staff members can provide insight into the quality of care provided by the nursing home. Testimonies from witnesses who observed neglect or poor treatment can significantly strengthen your case.
Preserving this evidence early is critical, as conditions can change rapidly. Collecting documentation, photos, and witness accounts as soon as possible increases the chances of building a solid case.
What Are Common Defenses Used by Nursing Homes in Bed Sore Cases?
Nursing homes often employ various defenses when faced with bedsore lawsuits. Understanding these common defenses can help you and your legal team prepare a strong counter-argument:
- Pre-Existing Medical Conditions: Nursing homes may argue that residents’ pre-existing health conditions caused them to develop bedsores. While some medical conditions can increase the risk that a patient may develop bedsores, proper care can still prevent bedsores.
- Unavoidable Bedsores: Some facilities claim bedsores were inevitable due to the resident’s immobility or overall health status. However, federal and state regulations require nursing homes to take preventive measures, and in most cases, bedsores are preventable with appropriate care.
- Family’s Involvement: Another defense might be that the family delayed or refused necessary medical interventions, impacting the resident’s health. This tactic shifts blame to the family, but a well-documented case can refute this argument, proving it was elder abuse.
Nursing Homes’ Bedsore Prevention Duties
To successfully pursue an elder abuse or bedsore lawsuit, you must prove that the nursing home’s negligence directly caused the development of the resident’s bedsores or worsened their condition.
Under 42 CFR § 483.25(c), nursing homes must ensure residents do not develop pressure ulcers unless they are clinically unavoidable. Demonstrating that the bedsores were avoidable and directly caused by the facility’s negligence is key to proving liability.
This involves demonstrating four essential legal elements: duty of care, breach of duty, damages, and causation.
Duty of Care
Nursing homes have a legal obligation to provide their residents with a standard level of care, as outlined under laws like the Federal Nursing Home Reform Act (42 CFR § 483.25), which mandates proper treatment, supervision, and care to prevent avoidable injuries, including bedsores.
This duty includes ensuring that residents receive adequate nutrition, regular repositioning to relieve pressure, and prompt medical attention by wound care specialists if bedsores develop. Establishing that the healthcare provider owed this duty is the foundation for any negligence claim.
Breach of Duty
A breach occurs when the nursing home fails to meet the legally required standard of care. Common breaches in bedsore cases include:
- Failing to reposition immobile patients regularly
- Inadequate staffing or supervision
- Neglecting to provide medical evaluations or necessary treatment
The breach must demonstrate that the nursing home’s actions (or inaction) were not what a reasonable facility would have done under similar circumstances, thus contributing to the development or worsening of bedsores.
Damages
Damages represent the harm suffered by the resident due to the facility’s negligence. In bedsore cases, damages often include:
- Physical pain and suffering
- Emotional distress
- Medical expenses for treatments like wound care, debridement, or hospital stays
The severity of the bedsores typically influences the potential compensation, with more severe injuries justifying higher awards.
Causation
Causation links the nursing home’s breach of duty directly to the resident’s bedsores. You must prove that the facility’s negligence was the primary cause of the injury rather than an unavoidable consequence of the resident’s underlying health conditions.
Nursing homes often argue that certain bedsores were inevitable due to conditions such as diabetes or immobility, making this element critical to establish through expert testimony and medical records.
What Is the Role of Expert Witnesses?
Expert witnesses play a critical role in bedsore lawsuits by helping to establish that the nursing home’s negligence led to the resident’s injuries. Typically, these experts are medical professionals who can testify that the bedsores were preventable with proper care.
They can explain how the nursing home’s failure to provide necessary medical treatment, reposition residents, or ensure adequate nutrition directly caused the development and worsening of existing bed sores.
Their testimony is often pivotal in showing that the nursing home or medical facility acted below the accepted standard of care, making it clear the injuries were a result of neglect and could have been avoided.
What Is the Statute of Limitations for Bed Sore Lawsuits?
The statute of limitations is the legal time frame within which a bed sore lawsuit must be filed. The statute of limitations varies by state but typically ranges from one to three years from when the injury was discovered or should have been found.
It is essential to act quickly, as filing after the statute of limitations expires will likely result in the dismissal of the case, regardless of its merits. A nursing home pressure injury attorney can help meet all legal deadlines, giving your family the best chance of pursuing justice.
What Compensation Is Awarded in Nursing Home Abuse Cases Involving Bed Sores?
When a resident suffers from bedsores due to neglect or improper care, the law allows victims and their families to seek financial compensation for the harm caused. The compensation awarded in cases involving bed sores typically falls into several categories, each designed to address different aspects of the suffering and losses incurred.
Economic damages cover the direct financial costs associated with developing and treating bedsores. These damages often include medical expenses, long-term care, and other costs tied to the resident’s recovery.
Non-economic damages address the emotional and physical suffering caused by the development of bedsores. This can include compensation for pain and suffering, loss of quality of life, and the psychological toll the injuries have taken on the resident.
Punitive Damages
In cases where the nursing home’s neglect was particularly egregious or intentional, punitive damages may be awarded. These damages are meant to punish the facility for its conduct and deter similar behavior in the future.
Wrongful Death Damages
If a resident dies due to complications from untreated bedsores, the family may be entitled to damages for funeral expenses, loss of companionship, and other related costs.
What Is the Average Payout for Nursing Home Decubitus Ulcers?
Payouts in nursing home bedsore cases range from $55,169 to $114,000,000. The average payout is $6,116,979, while the median recovery is $1,000,000.
Several factors can influence the value of a claim, including:
- Stage and severity of the bedsore and whether a serious infection, amputation, or death occurred
- Resident’s age, overall health, and life expectancy
- Whether the injury was preventable through repositioning, monitoring, or staff intervention
- Documentation of care plans, wound treatment, and whether records were falsified or incomplete
- Timing and quality of medical care provided once the sore was identified
- Evidence of systemic understaffing, poor training, or neglectful supervision
- Testimony from medical and nursing experts on causation and standard of care
Example Bed Sore Cases
$4,357,763 Verdict – Falls, Fractures, and Bed Sores caused by Nursing Home Negligence
Arcelia Martinez, 92, suffered from Parkinson’s, Alzheimer’s, and dementia. Despite being identified as a high fall risk, her nursing home allegedly failed to provide adequate supervision and staffing. She endured multiple falls, developed stage 2 bedsores that required multiple hospitalizations, which her family argued were a direct result of understaffing and neglect.
Staff allegedly failed to update records and communicate changes in her condition. Martinez later sustained a fall that fractured her leg. A jury awarded $4,357,763.40, including $4 million in punitive damages against the facility’s management company.
$1,434,600 Arbitration Award – Bed Sore Leads to Amputation
Gary Cinqmars, 64, entered a nursing facility for short-term rehabilitation but developed a pressure sore on his left heel within days. The wound worsened, became infected, and ultimately required a below-the-knee amputation. His attorneys argued the staff failed to implement basic wound prevention measures, monitor the sore, or refer him for vascular care despite his diabetes and vascular disease.
Records suggested little to no treatment was provided, and the ulcer rapidly deteriorated. An arbitrator found the facility mostly responsible and awarded $1,912,800, reduced to $1,434,600 after comparative fault.
What Factors Affect Compensation Amounts?
The compensation awarded in bedsore cases can vary widely depending on several critical factors, including the extent of the pressure ulcers. Each case is unique, and the specific circumstances surrounding the injury will influence the final compensation awarded. Below are some of the critical factors that affect compensation amounts in nursing home bed sore lawsuits:
Severity of the Injury
The extent of the bedsores plays a significant role in determining the compensation.
More severe cases, such as Stage 3 or Stage 4 pressure ulcers, typically result in higher compensation due to the increased pain, suffering, and need for long-term treatment. Severe bedsores can lead to serious complications such as infections, sepsis, and even death, which significantly increases the potential compensation.
Level of Negligence
Another important factor is the degree of neglect in the nursing home.
Suppose it can be proven that the nursing home repeatedly ignored signs of developing bed sores, failed to provide necessary care, or violated federal and state regulations. In that case, compensation amounts are likely to be higher. The more egregious the neglect, the greater the potential for punitive damages.
Impact on the Victim’s Life
Compensation is also influenced by how the bedsores have affected the victim’s quality of life.
For example, if the resident has endured significant pain, reduced mobility, or emotional trauma as a result of the pressure ulcers, non-economic damages may be substantial. Cases where the victim’s long-term health and well-being are compromised usually result in higher compensation.
Medical Records and Costs
The costs associated with treating bedsores, including hospitalization, surgery, medications, and ongoing care, are considered when determining compensation. The more extensive and long-lasting the treatment required, the higher the compensation awarded for economic damages.
Duration of Nursing Neglect
Another critical factor is the length of time the nursing home allowed the bedsores to progress without intervention. If the resident was left to suffer for an extended period, this could demonstrate severe neglect and risk of pressure ulcer development, warranting more significant compensation.
Other Contributory Factors
In some cases, nursing homes may argue that pre-existing conditions, such as vascular disease or other health issues, contributed to the development of bedsores.
While these conditions may influence the outcome, nursing homes must provide proper care to prevent bedsores from developing or worsening. How these contributory factors are addressed may impact the final compensation.
How a Bedsore Lawyer Can Help
When a loved one developed pressure injuries due to nursing home neglect, pursuing legal action can feel overwhelming. A skilled nursing home pressure ulcer attorney can provide the expertise and support needed to navigate the legal process.
From investigating the case to taking it to trial, a dedicated attorney will work to hold the nursing home accountable and secure fair compensation for the harm caused.
Investigating the Case
A pressure-sore attorney will thoroughly investigate the circumstances surrounding your loved one’s injury. This includes reviewing medical records, analyzing the nursing home’s care history, and identifying any instances of neglect or improper treatment.
By conducting a detailed investigation, your attorney can build a strong case demonstrating the facility’s failure to provide adequate care.
Gathering and Preserving Evidence
A crucial part of any bedsore lawsuit is gathering and preserving evidence that proves the patient suffered damages due to negligence. Your attorney will collect medical documentation, photographs of the bedsores, witness statements, and other relevant evidence to support your claim.
Preserving this evidence early on is essential for establishing the severity of the injury and the nursing home’s responsibility.
Negotiating with Insurance Companies
Nursing homes and insurance companies often attempt to minimize payouts in bedsore cases. An experienced bedsore lawyer will negotiate with insurance companies on your behalf, ensuring you receive a fair settlement covering all medical expenses, pain and suffering, and other damages.
Your attorney will use their expertise to push back against lowball offers and seek the compensation you deserve.
Bedsore Litigation in Court
If a fair settlement cannot be reached through negotiations, your attorney will be prepared to take the case to trial. A skilled nursing home pressure sore lawyer will present the evidence, call upon expert witnesses, and argue your case before a judge or jury to seek maximum compensation for your loved one’s suffering.
Consult Our Law Firm to Protect Your Legal Rights
If your loved one developed bedsores due to a healthcare provider’s negligence, you don’t have to face this battle alone.
At the Nursing Home Law Center, we have extensive experience handling cases involving decubitus ulcers and fighting for the rights of victims. Our law firm understands the unnecessary pain bedsores can cause and is committed to holding negligent nursing homes accountable.
Our dedicated team of bedsore lawyers is ready to help you pursue justice and secure the compensation your family deserves. We offer a free consultation to discuss your case and provide the guidance you need to take the next steps.
Don’t wait, and contact us today to learn how we can help you protect your loved one’s rights and seek financial compensation for their suffering. Let our nursing home abuse lawyers fight for the justice your family deserves. Call us or fill out our contact form.