Symptoms of Sepsis from UTI in Elderly Nursing Home Residents
Symptoms of sepsis from a UTI in elderly adults can include confusion, rapid breathing, an elevated heart rate, low blood pressure, fever, chills, weakness, and reduced urine output. In a nursing home, signs like these may suggest failures in monitoring, reporting condition changes, or obtaining timely treatment. Our nursing home sepsis lawyers stand with families dealing with this kind of harm. Contact us and seek justice for your loved one today.
What Is Urosepsis?
Urosepsis happens when a urinary tract infection (UTI) leads to sepsis. In older adults, this is a medical emergency because the infection can move beyond the urinary tract, trigger widespread inflammation, and cause organ damage, organ failure, or septic shock if treatment is delayed.
Urosepsis remains one of the leading forms of sepsis, with up to 30% of cases traced back to an infection in the urinary tract. Older adults and elderly patients face a higher risk of this progression, especially when they have a weak immune system, chronic diseases, kidney disease, or a urinary catheter.
What Is a UTI?
A urinary tract infection (UTI) is an infection anywhere in the urinary system, including the urethra, bladder, ureters, or kidneys. Most cases start in the bladder before the infection progresses.
UTIs are extremely common, and their prevalence rises with age. According to the National Institutes of Health, the incidence rate is 50−60% in adult women. In those over 65, the prevalence is approximately double that seen in the female population overall.
Common types of urinary tract infection include:
- Urethritis,
- Cystitis,
- Pyelonephritis, and
- Catheter-associated UTI.
What Is Sepsis?
Sepsis is a severe and life-threatening condition that happens when your body overreacts to an infection. Instead of fighting the disease, your immune system goes into overdrive and attacks your tissues and organs. This act can potentially lead to dangerously low blood pressure, organ failure, and, in the worst cases, sepsis can rapidly lead to death.
What Are the Symptoms of Sepsis From UTI in Elderly Adults?
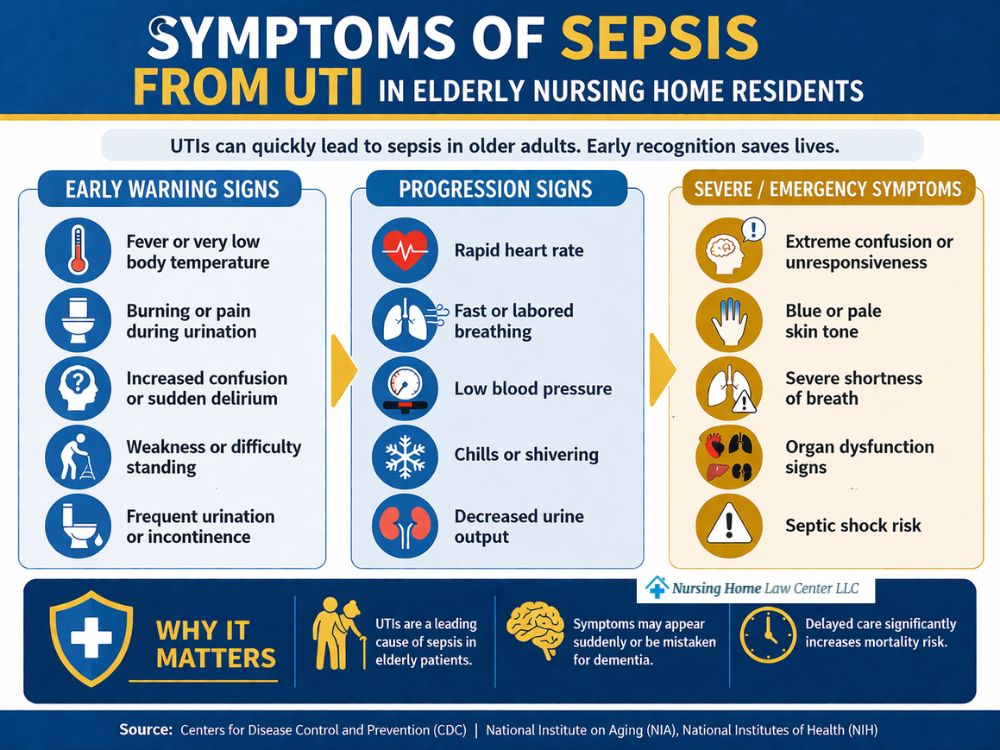
Common symptoms of sepsis from a UTI in elderly nursing home patients include:
- Sudden confusion or another change in mental status;
- Rapid breathing (faster than 22 breaths per minute);
- Rapid heartbeat;
- Low blood pressure (specifically, systolic blood pressure under 100 mmHg);
- Fever or chills;
- Weakness or unusual fatigue;
- Reduced urine output;
- Pale, clammy, or cool skin;
- Trouble breathing;
- A noticeable drop in alertness or responsiveness.
What Are the Symptoms of a UTI in Older Adults?
The typical UTI symptoms may also still be present at the same time, including:
- Painful urination;
- The urge to urinate frequently;
- Feeling an urgent need to go, even if there’s not much urine;
- Cloudy or bloody urine;
- Pelvic pain or pressure, especially in the lower abdomen;
- Urinary incontinence;
- In some cases, back pain if the infection reaches the kidneys.
Older adults might not always show these typical signs. Instead, they might experience less typical symptoms that can easily be mistaken for something else. For instance, they might suddenly become confused or agitated, show signs of lethargy, or even experience unexpected falls.
How Does a Urinary Tract Infection Lead to Sepsis?
When a UTI isn’t caught early, it can quickly become a much bigger problem, especially for older adults. What starts as a simple bladder infection can spread if left untreated. The bacteria can travel into the bloodstream, which is where things start to get dangerous.
Once the infection enters the bloodstream, it can trigger a systemic inflammatory response throughout the body. This response means the immune system goes into overdrive and tries to fight off the infection, but it ends up causing more harm than good. The body’s response can lead to tissue damage and, in severe cases, septic shock.
What Is Septic Shock?
The advanced stages of sepsis include severe sepsis or septic shock. That is the dangerous stage where the body can no longer deliver enough oxygen to major organs due to a drop in blood pressure. At that point, the risk of organ damage, organ failure, and other severe complications rises sharply.
Why Are Older Adults at a Greater Risk of Developing Severe Sepsis?
Older adults face a higher risk of developing severe-stage sepsis because age changes how the body responds to infection. Immune function tends to weaken over time, a process often described as immunosenescence, which can make it harder to contain a urinary tract infection before it spreads.
Older patients are also more likely to have multiple chronic conditions, reduced physiological reserve, and functional limitations that leave them less able to withstand a serious infection once sepsis occurs.
One systematic review reported that older adults are 13 times more likely to develop sepsis than younger adults and have a twofold higher risk of death from sepsis.
What Causes UTIs in the Elderly?
UTIs happen when bacteria or, in some cases, a fungal infection get into the urinary system and begin multiplying, most often in the bladder. For younger people, a UTI is often just a painful inconvenience, but for elderly patients, it can be much more severe.
An unmanaged or untreated UTI can lead to sepsis. The bacteria can spread beyond the urinary tract, enter the bloodstream, and cause a full-body inflammatory response that can be life-threatening.
What Are the Risk Factors for UTI in the Elderly?
Several risk factors make older adults more likely to develop a urinary tract infection and more likely to suffer serious complications if the infection is missed, including:
- Catheter use, which increases the chance that bacteria will enter the urinary tract;
- Kidney disease and other chronic diseases that affect how the body handles infection;
- Weakened immune systems, which can make it harder to fight off bacteria early;
- Immune suppression related to chemotherapy, organ transplant, or another serious medical condition;
- Conditions that reduce mobility, impair communication, or complicate recovery;
- Urinary incontinence, especially when hygiene care depends on staff response;
- Poor bladder emptying, which allows urine to remain in the bladder longer;
- A history of chronic or recurrent UTIs;
- Conditions such as chronic obstructive pulmonary disease and diabetes, which can leave an elderly person more medically fragile overall.
How Is Urosepsis Diagnosed?
Tests used to diagnose urosepsis may include:
- Complete blood count (CBC), which shows whether the body is responding to infection, including whether white blood cell levels are abnormal.
- C-reactive protein (CRP) or other inflammation markers to help providers identify inflammation and assess how serious the infection may be.
- Blood cultures to determine whether bacteria have entered the bloodstream and, if so, what organism is causing the infection.
- Blood tests to check organ function, damage, or failure.
- Urine testing and urine culture to confirm the presence of a UTI and identify the bacteria involved.
- Imaging studies, such as an ultrasound or CT scan to look for kidney infections, blockages, or other sources of infection in the urinary system.
In nursing home cases, diagnosis should begin as soon as a resident shows warning signs. Beyond what hospital providers found after transfer, our nursing home UTI lawyers also look at what the facility documented before that point. If a resident had clear symptoms of a UTI, early signs of sepsis, or a noticeable change in condition, the nursing home should have recognized the problem, notified the appropriate provider, and arranged urgent evaluation. When staff delay that response, the issue may support a nursing home abuse and neglect claim based on delayed treatment and missed warning signs.
How Is Urosepsis Treated?
Urosepsis treatment has to begin quickly and often includes:
- If doctors suspect sepsis, they usually prescribe antibiotics right away because early treatment can limit the infection from spreading further. Broad-spectrum antibiotics are often used first, then adjusted once blood cultures or a urine culture identify the bacteria causing the infection.
- IV fluids are commonly used to support circulation. They are especially important when the resident shows weakness or other signs that the infection is affecting the whole body.
- Some patients need oxygen if sepsis affects breathing.
- If fluids alone do not correct dangerously low blood pressure, providers may use additional medication to stabilize the patient.
- A resident with septic shock may need intensive monitoring to watch for organ damage, failure, or other serious complications.
- Providers may also need to address the underlying cause, including a blocked urinary tract, a contaminated urinary catheter, or a more advanced kidney infection.
In older adults, this is a medical emergency, not something providers watch for a day or two to see whether it improves on its own. Prompt treatment can make a substantial difference in whether the resident recovers without lasting harm. When treatment is delayed, the infection can continue to spread, leading to widespread inflammation, reduced blood flow to major organs, and an increased risk of life-threatening complications.
The Role of Nursing Homes in Preventing and Managing UTIs and Sepsis
Nursing homes play a big part in keeping older adults safe from UTIs and the dangerous possibility of sepsis. With proper care, many of the risk factors can be managed effectively.
Proper Hygiene and Infection Control Practices
Good hygiene is crucial. Regular cleaning and caring for residents help prevent future infections. Simple things like proper handwashing and keeping the urinary tract healthy can make a huge difference in avoiding infections.
Timely and Accurate Diagnosis and Treatment
Nursing home staff need to stay alert. Catching the symptoms of a UTI early means the difference between a quick fix and something much worse, like septic shock. Prompt treatment keeps the infection from spreading and causing more harm.
Adequate Staffing and Training
Having enough well-trained staff is important. Knowledgeable and attentive caregivers can spot problems early. This kind of care helps manage and reduce the risk of UTIs and sepsis.
Secure Expert Legal Representation
If you believe that your loved one has severe symptoms of a UTI or suspected sepsis due to nursing home neglect, it’s important to take action right away. The Nursing Home Law Center is here to help you understand your legal options.
Our nursing home negligence attorneys know how devastating it can be to see someone you care about being harmed by poor care, and we’re committed to holding those responsible accountable.
Contact us today for a free consultation at (800) 926-7565 or fill out our contact form. Our experienced team is ready to provide the support and guidance you need during this challenging time.
FAQ
Can a UTI cause sepsis in elderly residents with compromised immune systems?
Yes. A urinary tract infection can cause sepsis if the infection spreads beyond the urinary tract and triggers a severe response throughout the body.
Can a urinary tract infection be life-threatening in elderly adults?
Yes. In older adults, even a common infection can become a life-threatening condition if it is missed, left untreated, or allowed to progress into sepsis.
How long does it take for a UTI to turn into sepsis?
There is no fixed timeline. In some elderly patients, the infection progresses quickly, especially when the person has a weak immune system, multiple chronic conditions, or a catheter.
What are the early signs that a UTI might turn into sepsis?
Sepsis cannot go long unnoticed. Per the TIME initiative by the Sepsis Alliance, early warning signs can include sudden confusion, fever, chills, weakness, fast heartbeat and breathing, and blood pressure drops. In nursing home residents, a sudden decline in alertness or responsiveness also warrants immediate concern.
When does an elderly person need immediate medical attention?
An elderly person needs immediate medical attention if they have a UTI along with confusion, breathing changes, blood pressure drops, reduced urine output, extreme weakness, or any sign that the infection is spreading or becoming a medical emergency.

