The Nursing Home Law Center is committed to providing the legal resources necessary to hold negligent facilities accountable.
Bed Sore Stages
What Staging Reveals About Nursing Home Neglect
Summary:
Bed sores, also called pressure ulcers, are wounds that occur when constant pressure limits blood flow to the skin and tissue beneath it. In nursing homes, bed sore stages can say a lot about the quality of care a resident received.
If your loved one’s pressure sores have reached an advanced stage, we can help you protect their legal rights.
How Are Pressure Sores Staged?
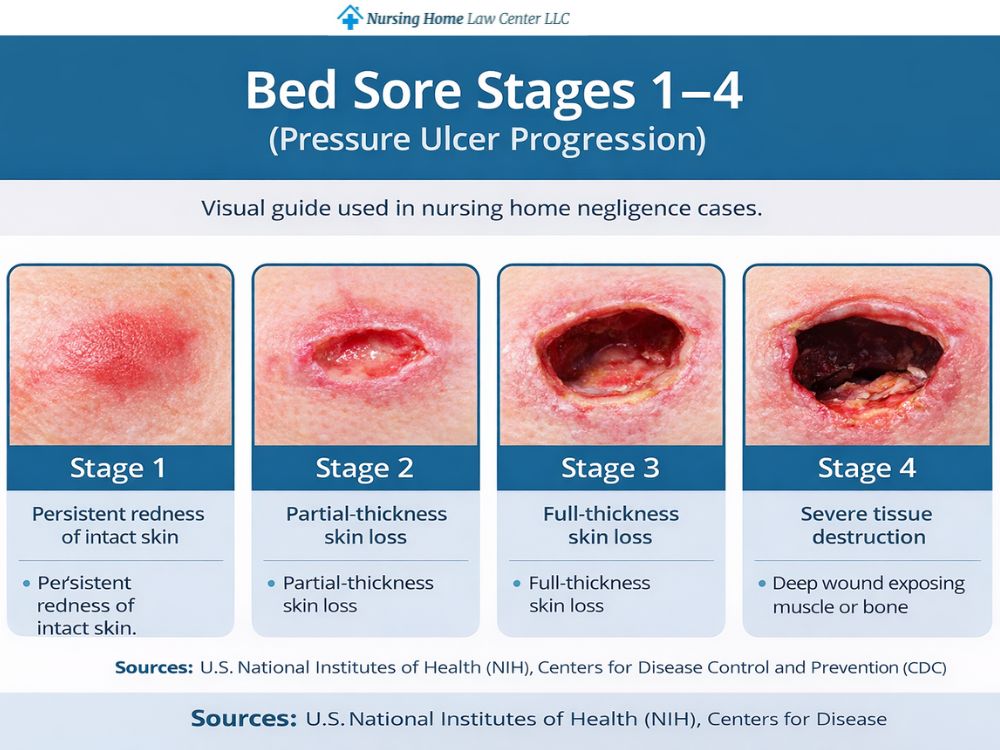
Doctors and wound care teams stage pressure ulcers based on how deeply the sore has damaged the skin and underlying tissue. The four stages help explain how bed sores look like as they worsen and which pressure sore symptoms tend to appear along the way.
Staging also helps guide treatment and gives healthcare providers a better sense of what care the resident needs.
Stage 1
At stage 1, the skin remains intact, but the affected area shows non-blanchable discoloration, meaning it does not turn white when pressed. On lighter complexions, it may look red. On darker skin color, it may appear purple, blue, or simply different in color from nearby skin. The spot may feel warmer or cooler than the surrounding skin and may feel firm or boggy.
Residents often report pain or itching before anything else becomes obvious. Staff should offload the area right away and arrange a same-day evaluation if the sore changes.
Stage 2
At stage 2, the damage has moved past surface irritation and created a shallow open wound or blister. The wound bed often looks pink or red, and the break in the skin raises the risk of bed sore infection.
At this stage, prompt care matters. Staff should keep the affected area clean, protect it from further pressure, and make sure the resident receives medical attention.
Stage 3
Stage 3 involves full-thickness skin loss. The sore often looks like a crater, and fat may be visible in the base of the wound. Slough may appear, although deeper structures are not yet exposed. This stage reflects serious damage from unrelieved pressure and often raises concerns about neglect.
A tunneling pressure wound may develop, creating hidden spaces beneath the edges of the wound that make care harder and raise the risk of infection.
Stage 4
Stage 4 is the most severe stage and can be extremely painful. The wound extends through the tissue and may expose or make it possible to feel deeper structures beneath the surface. Tunneling is common, and the risk of severe joint infections or bone infections, such as pressure ulcer osteomyelitis, rises sharply.
A pressure injury at this stage can trigger sepsis and quickly become life-threatening, especially for frail residents. In such cases, it is essential for families to speak with an elderly sepsis lawyer.
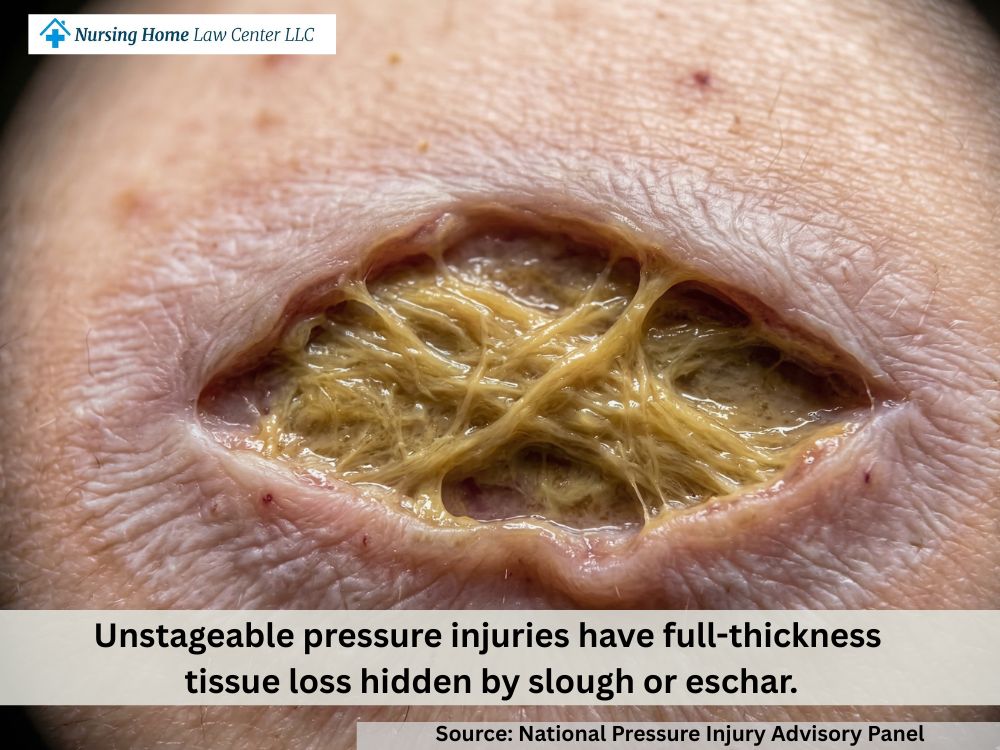
Unstageable Bedsores vs Deep Tissue Pressure Injury (DTPI)
An unstageable bedsore means the injury is clearly present, but no one can tell how deep the wound goes because the base is covered. That covering may be slough, which looks yellow or tan, or eschar, which appears black or brown and may include dead tissue. Until the covering is cleared away, the true depth of the wound stays hidden.
Many wounds first labeled unstageable later turn out to be skin ulcer stages 3 or 4.
A deep tissue pressure injury, or DTPI, starts below the surface. Pressure and shear can damage tissue near the muscle-bone interface before the skin even breaks open. That makes DTPI especially dangerous in a nursing home setting. These injuries can deteriorate quickly and later open into a more severe ulcer.
How Are Pressure Injuries Treated by Stage?
Treatment depends on how far the sore has progressed, the resident’s overall health, and whether staff respond to the first signs of a pressure injury in a timely manner.
- Stage 1: The focus is to reduce pressure, protect the skin, and watch for signs that the area is getting worse.
- Stage 2: Care usually includes moisture barrier creams and dressings such as DuoDERM for pressure ulcers, closer monitoring, and steps to lower the risk of infection.
- Stage 3: Deeper sores often need more aggressive pressure injury treatment, regular wound care, and evaluation for complications.
- Stage 4 or unstageable sores: Serious cases may involve infection control, specialty care, removing dead tissue or bedsore debridement, and sometimes require surgery.
How Nursing Homes Can Prevent Bed Sores From Advancing to Severe Stages
Advanced decubitus ulcer stages rarely result from one missed task. Usually, bed sores develop when staff repeatedly fail at following preventive measures and CMS pressure ulcer guidelines. Good nursing home care can interrupt that pattern. Staff need to identify vulnerable areas, respond quickly, and keep up the daily care that protects residents from prolonged pressure.
Keeping the Skin Clean and Treating Open Wounds
Poor hygiene in nursing homes often leaves residents exposed to preventable harm. Skin breaks down faster when it stays damp, soiled, or irritated. Once a sore opens, cleanliness matters even more. Staff need to keep the area dry, protect the surrounding skin, and provide consistent pressure wound care to promote healing.
Regular Skin Inspections of Areas Exposed to Prolonged Pressure
Bed sores often begin with subtle changes that are easy to overlook. Daily checks of the heels, hips, tailbone, elbows, and other high-risk areas give staff a chance to catch damage before the skin opens. These inspections matter even more for residents who cannot move easily or explain what they feel.
Frequent Repositioning to Relieve Pressure
Residents who remain in one position for too long need staff to move them often enough to ensure vulnerable areas sustain less pressure. That care must happen on schedule, not when someone gets around to it. Frequent repositioning helps ease pressure, protect blood flow, and keep a minor sore from becoming a deep wound.
Proper Nutrition and Hydration
Malnutrition in nursing home residents slows recovery and leaves the skin more fragile. Staff should notice weight loss, poor appetite, and signs of dehydration in nursing home patients before those problems begin affecting the bedsore.
What Bed Sore Stages Can Reveal About Nursing Home Care
The stages of bed sores can reveal a great deal about the care a resident received. In a nursing home, an advanced pressure ulcer often points to breakdowns in staffing, communication, follow-through, or basic care. A nursing home pressure ulcer lawyer can help prove neglect contributed to the resident’s injuries.
How Nursing Home Law Center Can Help
Pressure ulcers leave a paper trail, showing whether the nursing home responded appropriately or let the sore worsen. Our law firm can review turning and repositioning logs, care plan notes, skin assessments, charted changes, wound measurements, staging records, and dated photographs. We can also examine mattress or cushion orders, heel protection, wound-care consult timing, infection workups, and hospital transfers.
Our nursing home abuse lawyers have successfully recovered bedsore settlements for families after nursing homes failed to prevent pressure injuries or treat them properly.
- $3,000,000: Sharon’s husband entered a skilled nursing facility after hip replacement surgery. During his stay, he developed severe pressure ulcers, and staff missed signs of infection as his condition worsened. He later died. The value of the case reflected the wrongful death, the extent of the wound progression, and the evidence of missed care during recovery.
- $1,095,000: Debra, a sixty-two-year-old woman, entered a nursing home for rehabilitation after hip replacement surgery. Staff failed to get her out of bed at the intervals her doctor ordered, and she developed serious pressure ulcers on her buttocks. Her injuries required multiple debridements and flap reconstruction surgery, both of which affected the value of the case.
FAQs
What are the risk factors of developing pressure sores?
Elderly nursing home residents who are most at-risk of developing bed sores include those with limited mobility, long periods in bed or a wheelchair, poor nutrition, dehydration, incontinence, reduced sensation, and medical conditions that affect circulation. Frail residents, particularly those who depend on staff for changing position, turning, bathing, and toileting, face a much higher chance of developing a pressure sore when daily care slips.
How long do bedsores take to develop?
How fast bedsores develop depends on the resident’s overall condition. A resident who has poor circulation or needs full assistance with daily care may develop a pressure sore much faster than a healthier, more mobile person.
How long do pressure ulcers take to heal?
Wound healing depends on pressure relief, nutrition, and the quality of care. However, infections or certain conditions, such as diabetes, can affect recovery time. Early stages of pressure sores may heal completely in weeks, while deeper sores can take months to heal and may never fully close in a frail nursing home resident.
Where do bedsores progress the fastest?
Bedsores tend to worsen in areas where the skin covers bone with very little cushioning. The most common areas for bed sores are the tailbone, hips, heels, ankles, and elbows.