legal resources necessary to hold negligent facilities accountable.
Towson Nursing Home Abuse & Neglect Attorneys
Nursing home residents are tragically susceptible to abuse and neglect, leading to severe injuries and, in extreme cases, death. These incidents reveal a distressingly lacking proper care and attention in facilities meant to be safe havens for the elderly.
Nursing Home Law Center, LLC provides crucial assistance and information to victims of nursing home abuse, aiding them in their quest for justice. Our nursing home abuse lawyers work diligently to secure compensation and enforce accountability for the harm caused to our clients.
Prevalence of Abuse in Towson Nursing Homes
The prevalence and seriousness of nursing facility abuse and neglect in Towson, Maryland, are alarming concerns. Being a bustling suburb of Baltimore County, Towson has numerous nursing and assisted living facilities. Recognizing and addressing this issue is not just a legal matter but a moral imperative.
Towson's nursing home patients are entitled to legal protections and rights, ensuring their safety and well-being. As attorneys specializing in elder care abuse, our law offices in Baltimore City are dedicated to defending these rights and providing legal recourse to victims and their families.
CMS Nursing Home Statistics
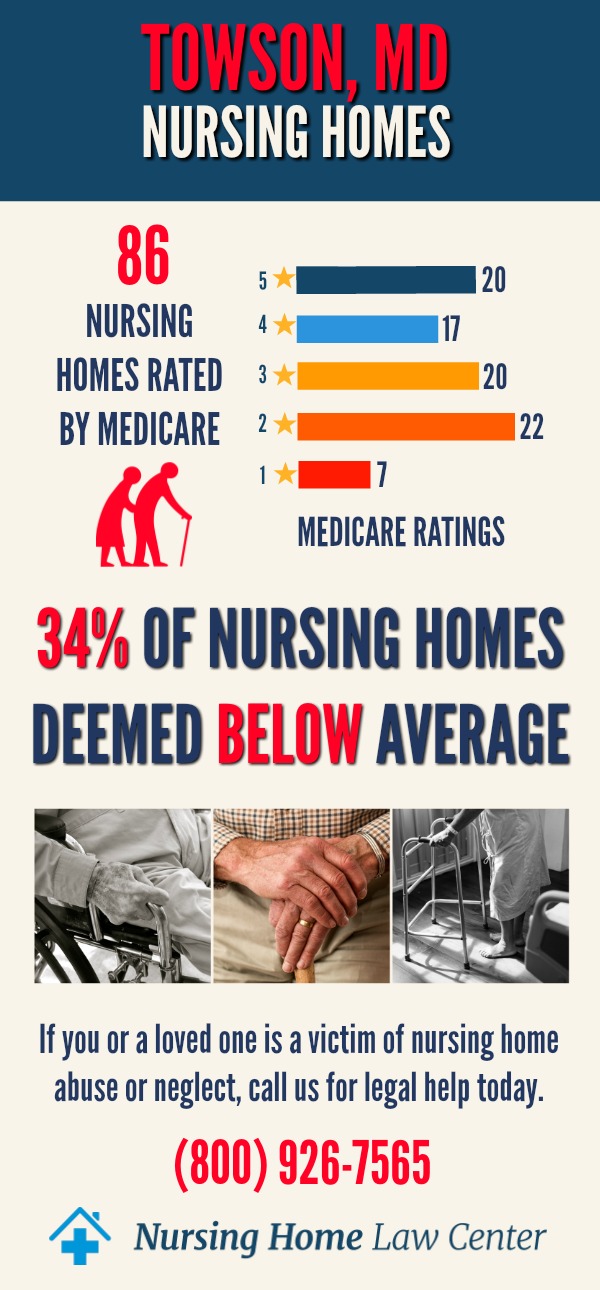
In January 2024, the Centers for Medicare and Medicaid Services (CMS) conducted a comprehensive assessment of nursing homes in Towson, Maryland. This evaluation revealed a concerning statistic: out of the 94 nursing facilities assessed in the area, 41 of them, which accounts for 44%, were rated as "below average" or "much below average."
This rating suggests potential issues with the quality of care provided to Towson patients in a nursing home or assisted living facility.
Maryland Nursing Home Facilities Cited for Abuse
Inspectors identified several nursing homes in Towson that have been cited for abuse during the CMS evaluation. Here is a list of these facilities, alphabetized and in title case:
- Autumn Lake Healthcare at Glen Burnie
- Autumn Lake Healthcare at Summit Park
- Autumn Lake Healthcare Post Acute Care Center
- Carroll Park Health Care
- Ellicott City Healthcare Center
- Northwest Health Care Center
- Oakwood Skilled Nursing Facility
- Forest Haven Nursing and Rehabilitation Center
These nursing homes have been under scrutiny due to reports of abuse, highlighting the significance of government agencies' efforts to maintain high standards of care in nursing facilities.
Definition and Types of Abuse
In Towson, abuse in nursing homes takes various forms, each with severe consequences for the victims.
- Physical Abuse: The deliberate application of force that results in pain, injury, or emotional distress to an individual in a nursing home or assisted living facility.
- Sexual Abuse: Any form of coerced or non-consensual sexual contact or interaction by the nursing home staff, visitor, family member, or other nursing home resident.
- Emotional and Psychological Abuse: Engaging in verbal or nonverbal actions that lead to mental anguish or suffering.
- Financial Abuse: Unauthorized or illegally exploiting an elder's financial resources or property.
- Nursing Home Negligence: The omission of essential care, leading to the failure to satisfy the fundamental needs of elderly individuals.
- Medical Malpractice: Negligence in medical care, notably in failing to diagnose conditions, potentially leading to injury or death.
Identifying Abuse in a Maryland Nursing Home
Recognizing the signs of abuse, mistreatment, and neglect is critical in protecting nursing home patients.
- Signs and Symptoms: Physical and behavioral indicators, such as unexplained injuries,pressure ulcers, and changes in mood or behavior, can be signs of abuse or neglect. These symptoms require immediate attention and investigation.
- Legal Framework for Abuse Recognition: Understanding the legal definitions and criteria for identifying abuse is essential. Our law offices are proficient in interpreting these criteria and applying them to protect the rights of Maryland nursing home residents.
Reporting Abuse in Maryland Nursing Homes
However, when the shadow of abuse, mistreatment, and neglect creeps into these havens, it's not just the immediate injury to the resident that raises alarm. The unreported mistreatment can be a silent predator, potentially escalating to more severe harm or even death.
Reporting such incidents is a crucial mechanism for protection—it acts as a safeguard for the victim and the entire facility's community. A care plan interrupted by abuse is a failed plan.
Families in Maryland entrust their loved ones to the care of professionals, believing in a promise of safety and comfort. When that trust is broken, reporting by families, hospital staff, or a lawyer triggers an investigation, stopping the cycle of pain and ensuring the residents' dignity is restored and preserved.
You can report nursing facility abuse to the following agencies:
- Maryland Department of Human Services - Adult Protective Services
- National Center on Elder Abuse (NCEA)
- Long-Term Care Ombudsman
Our Legal Approach to Maryland Nursing Facility Abuse Cases
Our law firm employs thorough investigative techniques, including in-depth interviews and meticulous medical and facility records analysis. This approach helps us uncover the truth and build a strong case for our clients.
We apply Maryland state laws effectively in abuse cases, ensuring that all legal avenues are explored to hold responsible parties accountable and seek justice for our clients.
Proving Maryland Nursing Home Neglect and Liability
Our legal team is adept at demonstrating how nursing care homes have failed in their duty of care and how these breaches have harmed or injured residents.
We specialize in illustrating the connection between negligent acts and the resulting harm, which is crucial in legal proceedings for abuse cases.
Maryland Nursing Home Victim and Family Support Services
We provide comprehensive legal counseling and support services for victims of nursing facility abuse and their families in Towson. Our team is committed to guiding them through the complexities of the legal process, ensuring they understand their rights and options.
Pursuing Justice and Compensation
Filing a lawsuit for nursing home neglect or abuse is a significant step toward obtaining justice and compensation for victims. We guide our clients through this process, ensuring they are informed and supported at every stage.
Our Maryland nursing home legal team is experienced in navigating settlement negotiations and trial processes. We work diligently to secure fair and just compensation for our clients through out-of-court settlements or courtroom advocacy.
Why Choose Our Towson Nursing Home Abuse Lawyers to Advocate for Your Loved Ones
Choosing our law firm means selecting a team with expertise, experience, and a client-focused approach. We understand the nuances of nursing home cases in Towson and are committed to achieving the best possible outcomes for our clients.
Next Steps After Contacting Us
Upon contacting our office, clients can expect a thorough evaluation of their case, compassionate legal advice, and a clear action plan. Our team prioritizes the well-being of our clients and their loved ones, ensuring their needs are met throughout the legal process.
Restoring Dignity: Legal Advocacy in Maryland Nursing Facility Abuse Cases
Has abusive behavior or negligence affected you or a loved one? If so, taking action is crucial. Nursing Home Law Center, LLC specializes in providing compassionate and effective legal advocacy to those who have suffered in nursing care homes.
Our experienced Maryland attorneys are dedicated to restoring dignity and seeking justice for our clients. Our services include:
- Expert legal counsel and advice
- Aggressive representation in and out of court
- Assistance with documentation and evidence gathering
- Persistent pursuit of fair compensation and justice
Contact our nursing home abuse attorneys at (800) 926-7565. We offer a free consultation and work on a contingency fee basis, prioritizing your peace of mind and legal success.
 Chicago Nursing Home Injury Attorney Nursing Home Law Center LLC Home
Chicago Nursing Home Injury Attorney Nursing Home Law Center LLC Home
