legal resources necessary to hold negligent facilities accountable.
Charleston Nursing Home Abuse Lawyer
 The Issue of Nursing Home Abuse is Alarmingly Prevalent, Often Hidden Behind Closed Doors of Care Facilities. Mistreatment Can Take Many Forms, Including Sexual Abuse, Neglect, Physical Harm, and Financial Exploitation, Leaving Lasting Damage on Its Victims.
The Issue of Nursing Home Abuse is Alarmingly Prevalent, Often Hidden Behind Closed Doors of Care Facilities. Mistreatment Can Take Many Forms, Including Sexual Abuse, Neglect, Physical Harm, and Financial Exploitation, Leaving Lasting Damage on Its Victims.
At Nursing Home Law Center, LLC, Our Legal Team is Adept at Uncovering and Bringing These Hidden Abuses to Light. Our Charleston Nursing Home Abuse Law Firm Strives to Provide Compassionate and Aggressive Representation to Achieve Justice and Fair Compensation for Our clients.
The Distressing Reality of Nursing Facility Abuse in CharlestonIn Charleston, the Grim Reality of Nursing Home Abuse is a Pressing Concern. Elderly Residents in These Nursing Homes, Who Should Be Living Their Twilight Years in Comfort and Dignity, Are Unfortunately Facing Varying Degrees of Mistreatment. Nursing Home Abuse in Charleston is Not Just Limited to Physical Harm. it Includes a Spectrum of Mistreatment That Significantly Affects the Physical, Emotional, and Financial Well-being of Elderly residents.
Prevalence and Impact of Abuse on SeniorsThe Prevalence of Abuse in These Settings is Alarming, With Incidents Ranging From Physical and Emotional Abuse to Neglect and Financial Exploitation. These Acts Not Only Breach the Trust Placed in Nursing Facilities but Also Leave Lasting Impacts, From Physical and Psychological Abuse to Diminished Trust and Security Among the Victims and Their families.
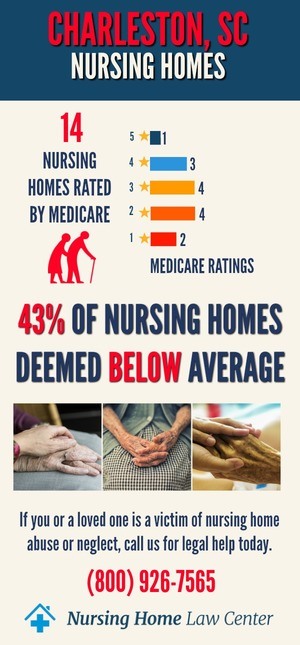
Alarming Statistics in Charleston, South Carolina Nursing HomesRegarding the Quality of Care in Nursing Homes, the Centers for Medicare and Medicaid Services (CMS) Statistics Reveal a Concerning Reality in Charleston, South Carolina. These December 2023 Statistics Indicate That a Significant Portion of the Nursing Homes in This Area, Precisely Seven Out of 17, Are Rated As "below Average" or "Much Below average."
This Rating Reflects the Urgent Need for the Following:
- Improved oversight
- Better Standards of care
- Increased Attention to the Well-being of Nursing Home residents
The Substandard Ratings Raise Questions About the Quality of Care and Safety Provided to Vulnerable Nursing Home patients.
The Call for ReformIn Light of These Statistics, There is a Pressing Need for Nursing Home Reform to Ensure That Residents Receive the Care and Respect They Deserve. Instances of Nursing Home Abuse, Neglect, Physical Abuse, Financial Exploitation, and Other Forms of Mistreatment Underscore the Urgency of This matter.
Families and Loved Ones Must Remain Vigilant, Recognizing the Common Signs of Abuse and Advocating for the Rights and Well-being of Nursing Home Residents. the Role of a South Carolina Nursing Home Neglect Attorney is Crucial in Bringing These Issues to Light and Seeking Justice for the victims.
 Identifying Nursing Home Neglect and Abuse
Identifying Nursing Home Neglect and AbuseIdentifying Nursing Home Abuse and Neglect is the First Step in Combating This Issue. it Requires a Keen Eye and Understanding of This Abuse's Various Forms. Recognizing the Signs Early Can Be Pivotal in Preventing Further Harm to Elderly Loved ones.
Warning Signs Indicative of Abuse or NeglectWarning Signs of Nursing Home Abuse and Neglect Can Be Both Overt and Subtle. They Include Unexplained Injuries, Sudden Behavioral Changes, and Unusual Financial Transactions. These Signs Call for Immediate Investigation to Protect the Nursing Home Patient From Further harm.
Different Forms of AbuseRecognizing the Different Types of Abuse and Their Signs and Being Vigilant When Visiting Loved Ones in Care Facilities or Dealing With Caregivers is Essential. Nursing Home Abuse Manifests in Various Forms, Each With Specific indicators.
Physical Abuse
Physical abuse could involve forceful bodily harm that might include the following:
- Unexplained bruises, cuts, or injuries.
- Broken bones or fractures.
- Evidence of restraints or excessive use of physical conditions.
- Fear or withdrawal when approached by specific individuals.
- Reports of being hit, slapped, or physically harmed.
Emotional abuse often inflicts psychological suffering and may exhibit these signs:
- Sudden changes in behavior, such as depression or withdrawal.
- Anxiety, fear, or nervousness, particularly in the presence of certain individuals.
- Low self-esteem and self-worth.
- Social isolation and withdrawal from family and friends.
- Verbal abuse, including insults, threats, or humiliation.
Sexual assault involves non-consensual sexual acts and may manifest through these indicators:
- Physical signs of sexual abuse, such as unexplained bleeding or pain.
- Fear or discomfort when discussing or being around the alleged perpetrator.
- Sexual behavior or knowledge beyond the individual's capacity or age.
- Changes in mood or behavior, including depression, anxiety, or withdrawal.
- Reporting inappropriate sexual contact or advances.
Financial abuse entails the exploitation of financial resources and may be evidenced by:
- Unexplained or sudden changes in financial documents, such as wills or power of attorney.
- Unexplained withdrawals from bank accounts or missing funds.
- Evidence of coercion or manipulation regarding financial matters.
- Changes in financial decision-making capacity.
Medical malpractice relates to substandard medical care and may involve:
- Failure to provide appropriate medical care or treatment.
- Medication errors, including incorrect dosages or medications.
- Unexplained or worsening medical conditions.
- Delayed diagnosis or treatment of medical issues.
- Lack of informed consent for medical procedures.
Neglect results from the failure to provide adequate care and might be indicated by:
- Signs of poor hygiene, such as dirty clothing or unclean living conditions.
- Untreated medical conditions lead to complications.
- Malnutrition or dehydration.
- Falls or accidents due to inadequate supervision.
- Pressure ulcers (bedsores) or infections from neglect of personal care.
Reporting any suspected abuse or neglect promptly is crucial to protect the well-being and rights of vulnerable individuals in caregiving settings.
Legal Rights and Protections for Nursing Home ResidentsResidents of nursing homes in Charleston, and by extension in South Carolina, are protected by many legal rights and safeguards. These protections ensure their safety and dignity within the nursing home setting.
Nursing home patients in Charleston are entitled to rights that safeguard their well-being. Violations of these rights necessitate legal intervention. These include the right to be free from the following:
- Abuse and neglect
- The right to privacy
- The right to receive adequate medical services, treatment, and ongoing care
State laws set strict standards for operations, including staff members' qualifications and nursing home resident protections. These regulations aim to protect and create a safe environment for nursing residents, ensuring they receive the care and respect they deserve.
Causes of Nursing Home Negligence and AbuseUnderstanding the underlying causes of nursing home abuse and neglect is essential for prevention and intervention. These causes are often complex, involving various systemic issues within Charleston nursing home facilities.
Systemic Issues Leading to Abuse and NeglectFactors such as understaffing, inadequate training, and the inherent vulnerability of seniors contribute to the prevalence of nursing home abuse. Addressing these systemic issues is critical in creating safer environments for our elderly population.
- Understaffing: Insufficient staff members can lead to neglect, as residents may not receive the required attention and care (medical malpractice).
- Lack of Training and Supervision: Inadequate training and supervision of staff members can result in improper care and failure to identify signs of abuse or neglect.
- Lack of Respect and Dignity: A disregard for residents' dignity and rights can contribute to mental abuse and diminish their overall well-being in nursing homes.
- Healthcare Fraud: Fraudulent activities within healthcare facilities can divert resources from residents' care, leading to neglect.
- Neglect Claims: Neglect claims may be ignored or downplayed by the facility responsible for the resident's care.
- Lack of Immediate Attention: Failure to address residents' needs immediately can lead to their suffering and even place them in immediate danger.
- Same Signs of Nursing Home Abuse or Neglect: Some signs of elder abuse or neglect may overlap, making it challenging to identify the specific issue.
- Family Member Concerns: Crises raised by family members may not be taken seriously or addressed promptly.
- Personal Property: Theft or mismanagement of residents' personal property can impact their quality of life.
- Medical Treatment: Adequate medical treatment may be delayed or denied, exacerbating residents' health issues.
When residents in nursing homes experience mistreatment, it can have severe and tragic consequences, including wrongful death. Nursing homes are meant to be places of care, comfort, and safety for elderly individuals who require assistance with their daily needs. However, instances of physical assault, sexual abuse, or neglect can jeopardize the lives of residents and result in devastating outcomes.
Recognizing the Warning SignsFamily members who have loved ones residing in nursing homes must remain vigilant about the potential for abuse and neglect. It is essential to be aware of the not-so-envious signs that may indicate abuse or neglect is occurring within the facility. These signs can include unexplained injuries, changes in behavior, sudden weight loss, or the development of bedsores.
Physical abuse can lead to severe injuries or exacerbate existing medical conditions, ultimately resulting in a preventable death. Similarly, sexual assault is a reprehensible violation of trust and can have lasting physical and emotional consequences. Neglect, whether intentional or due to inadequate care, can lead to preventable deterioration in health and, in the worst cases, preventable death.
Seeking Justice for Charleston Nursing Home Abuse VictimsSeeking justice for Charleston nursing home abuse and neglect victims is a pivotal aspect of addressing this issue. Legal action not only brings relief to the victims and their families but also serves as a deterrent against future instances of abuse.
Charleston nursing home abuse lawyers play a vital role in advocating for the rights of abuse victims. They provide legal expertise, represent the victims in court, and work tirelessly to ensure justice.
Filing Civil Lawsuits for Charleston Nursing Home Abuse and NeglectFiling a lawsuit for nursing home abuse or neglect involves navigating complex legal processes to prove abuse or neglect. Victims can claim damages for physical and emotional suffering, financial losses, and sometimes punitive damages.
What to Do if You Suspect Nursing Facility AbuseIf you suspect nursing home abuse, taking prompt and decisive action is crucial. This involves gathering evidence, ensuring the victim's safety, and reporting the abuse to the relevant authorities.
In cases of suspected abuse, immediate steps include:
- Documenting the abuse
- Removing the victim from the harmful environment
- Reporting to agencies like Adult Protective Services at the South Carolina Department of Social Services
- Legal counsel should be sought to navigate the complexities of the situation
- Contacting the Charleston Long-Term Care Ombudsman Program at (800) 868-9095
Ensuring the safety and dignity of elderly individuals in nursing homes is paramount. Our law firm plays a critical role in this endeavor, offering expert legal counsel and representation to victims of nursing home abuse and their families.
Protecting our loved ones in nursing homes is not just a legal obligation but a moral imperative. Our firm stands committed to this cause, offering our expertise and resources to those affected by nursing home abuse and neglect in Charleston.
Achieving Resolution and PreventionLegal action against nursing home abuse perpetrators and facilities plays a critical role in preventing future abuse. It brings accountability to the facilities and helps in implementing stricter safety measures.
Successful legal cases set a precedent, encouraging nursing homes and assisted living facilities to uphold higher standards of care. They also serve as a warning to potential abusers, thereby contributing to the overall safety of Charleston nursing home environments.
Protecting Your Loved Ones: Partnering With Charleston Nursing Home Abuse LawyersPartnering with a nursing home abuse lawyer is a crucial step in protecting your loved ones from abuse. Our Charleston nursing home abuse law firm is committed to providing expert legal assistance to abused victims, ensuring their rights are upheld and they receive the justice they deserve.
Our law firm specializes in nursing home abuse cases, offering comprehensive legal support from investigation to litigation. Our Charleston nursing home abuse lawyers is dedicated to safeguarding the rights of the elderly and ensuring they receive the respect and care they are entitled to.
If you suspect that a loved one is suffering from nursing home neglect or abuse in Charleston, don't stand by in silence. Nursing Home Law Center, LLC is your staunch advocate, ready to tackle nursing home abuse cases diligently and compassionately.
Our Charleston nursing home negligence law firm offers:
- Free consultation to discuss your concerns.
- A comprehensive investigation into abuse and neglect at nursing facilities.
- Legal pursuit of compensation for injuries, including broken bones.
- Ensuring that staff members responsible for abuse and neglect are held accountable.
- Zero fees until we win or settle your case.
- Accountability measures against staff members where neglect occurs.
If the signs of abuse or neglect are immediately apparent, contact us to pursue compensation. Your loved ones deserve a safe living environment; our competent personal injury law firm is here to ensure they get it. Call our nursing home abuse attorneys at (800) 926-7565.
 Charleston County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
Charleston County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
