legal resources necessary to hold negligent facilities accountable.
Jersey City Nursing Home Abuse Lawyer
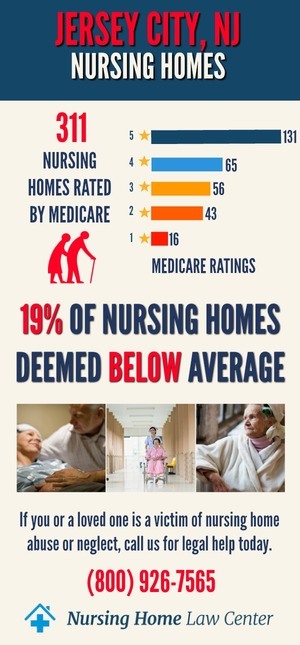 Abuse in Jersey City nursing homes is just as big of a problem as in other parts of the country. You should consult our lawyers to get justice if you or a loved one is abused in a New Jersey nursing home.
Abuse in Jersey City nursing homes is just as big of a problem as in other parts of the country. You should consult our lawyers to get justice if you or a loved one is abused in a New Jersey nursing home.
Were you or your loved one abused in a nursing facility? If so, the affiliate New Jersey personal injury attorneys at Nursing Home Law Center, LLC will assist you in filing a claim against the at-fault nursing home facility and its employees. We have successfully represented numerous clients in lawsuits against Jersey City nursing homes.
You can receive a free consultation from our NJ nursing home abuse lawyer to understand your legal options. Contact the Jersey City nursing home abuse lawyers at (800)-926-7565 (toll-free phone number) today to schedule a free case review to discuss a financial compensation claim.
 What is Nursing Home Abuse?
What is Nursing Home Abuse? The World Health Organization (WHO) defines nursing home abuse as a single or repeated act or lack of appropriate action occurring within any relationship where there is an expectation of trust which causes harm or distress to a vulnerable adult.
There are four main types of nursing home abuse: physical, sexual, emotional/psychological, and financial. The staff or other nursing home residents can be the responsible parties in a nursing home abuse case.
The WHO reports elder abuse in nursing homes can lead to long-term psychological and physical injuries. When your loved one does not get quality care at a facility, it can complicate their existing medical problems or result in significant emotional distress.
Likewise, if a nursing home resident is financially abused, they can lose their life savings or become bankrupt.
 What are the Signs of Abuse in Nursing Homes?
What are the Signs of Abuse in Nursing Homes? The signs of abuse can vary depending on its type. However, there are some general signs of nursing home abuse and neglect that you should be aware of:
- Unexplained injuries
- Broken bones
- Bruises
- Sprains
- Cuts
- Head injuries
- Black eyes
- Weight loss
- Dehydration
- Genital injuries
- Malnutrition
- Dirty clothes or bedding
- Unsanitary living conditions
- Pressure ulcers or bed sores
- Complicated medical conditions
- Soiled linens
- Infestation of insects or rodents
- Unusual behavior changes
Negligence by the nursing home staff can also lead to the resident's wrongful death, especially if they have dementia or another cognitive impairment.
Do you suspect your loved one is the victim of nursing home abuse and neglect? If so, contact the authorities immediately, then call our experienced Jersey City nursing home abuse lawyer affiliates to help investigate the situation and take legal action to get justice.
 What are the Most Common Types of Abuse in Jersey City Nursing Homes?
What are the Most Common Types of Abuse in Jersey City Nursing Homes? Residents in nursing home facilities can encounter different types of abuse. The common ones are the following.
Physical Abuse
Physical abuse can be defined as using physical force that may result in bodily injury, physical pain, or impairment. This abuse can involve
- Hitting
- Kicking
- Shoving
- Slapping
- Shaking
- Burning
- Bodily harm
Sexual Abuse
Sexual elder abuse is any non-consensual sexual act with residents. Caregivers, other residents, or visitors can take advantage of your loved one. Below are some warning signs to look for if you suspect someone you know has been abused sexually.
- Withdrawn demeanor
- Urinary Track infection
- Sudden transmission of an STD
- Timid attitude when in the presence of their abuser
- Skin tearing around genitals
Did you notice these signs in addition to bruises around your loved one's breasts or genitals? This indicator could signify sexual abuse, and you should contact the authorities to get it reported and a nursing home abuse attorney as soon as possible.

Emotional Abuse
Emotional elder abuse can involve verbal assaults, threats, intimidation, and emotional manipulation by staff or other residents. It may also include social isolation as a form of punishment.
Unfortunately, psychological abuse is the most common type of elder abuse in nursing home facilities. It mainly occurs because the facility is understaffed or the staff is not adequately trained to care for the elderly.
According to WHO data, psychological abuse is reported by 11.6% of the elderly at assisted care facilities. More than one in every ten individuals is abused while under professional care.
The consequences of psychological abuse can be just as damaging as bodily abuse, yet it often goes unnoticed and unreported. Victims of psychological abuse may suffer from anxiety, depression, sleep disorders, and low self-esteem.
Financial Abuse
Financial abuse refers to the unauthorized taking of a nursing home resident's money or property, such as valuables.
Signs of elder abuse in long-term care homes can be challenging to identify because the residents may be afraid to speak up or may not even know that what's happening to them is abuse.
Nursing Home Neglect
Nursing home neglect is also considered a form of abuse as it is the failure of facility staff to provide nursing home residents with the necessities of life, such as food, water, and clothing.
Prolonged cases of nursing home neglect can result in wrongful death. If a resident dies under suspicious circumstances, it is essential to gather witness statements or names and photographic evidence. Contact the proper authorities and someone you can trust to represent your loved one's rights.
Nursing home neglect can be challenging to gather evidence for since it is the absence of care. So, having a local abuse and neglect attorney to reference their knowledge and contact references to get the evidence needed to build a case against your perpetrator.
 How can a Nursing Home Abuse Attorney Help?
How can a Nursing Home Abuse Attorney Help? A nursing home that has been consistently causing neglect to a resident might not help find the perpetrator. Instead, in nursing home neglect cases, the perpetrator or facility is more motivated to save money or protect their reputation.
Our affiliate New Jersey Nursing home attorneys will investigate and represent your case under every aspect of the law and ensure that those responsible are held liable. You should also contact the police or an ombudsperson to validate the nursing home neglect claim and start a record of incidence in the case of additional events or wrongful death.
An experienced lawyer can help you by:
Filing a Personal Injury Claim
A personal injury is a physical or psychological harm caused by someone else's negligence or ill intent. When an elderly person is neglected, and it results in damages, the facility could be held liable.
You will need to prove that a Jersey City facility was aware of the abuse, did not take steps to prevent it and that your loved one was injured directly. Our experienced personal injury lawyers can help create a case if your loved one died unexpectedly or experienced life-altering injuries.
We'll collect sufficient evidence to prove your claim and get you the maximum recovery for your personal injury case.
Recover Damages
Residents suffering neglect at nursing homes or other care facilities can recover economic and non-economic damages for their injuries and, in some cases, wrongful death. Your loved one can claim for:
- Medical expenses
- Mental anguish
- Pain and suffering as a result of neglect
- Disability or impairment
- Loss of consortium
- Punitive damages in some cases
- Recover costs of care
Schedule a free consultation from our nursing home abuse attorney to receive justice for your loved one in a New Jersey assisted care facility.
 Hire a Jersey Nursing Home Abuse Attorney to Resolve Your Personal Injury Claim
Hire a Jersey Nursing Home Abuse Attorney to Resolve Your Personal Injury Claim Nursing Home Law Center, LLC has helped thousands of clients recover the compensation they deserve following negligent treatment or abuse at a long-term care center.
Do you suspect your loved one is a victim of abuse and neglect? Call us at (800) 926-7565 to arrange a free consultation with one of our affiliate Jersey City nursing home abuse attorneys. We can collect the information we need to begin a thorough investigation into the matter and review your legal options with you.
All nursing home negligence cases are handled on a contingency fee basis in Jersey City and additional locations. If we are unable to secure compensation on your behalf, our services will be free of charge. Talk to an experienced personal injury attorney today for a free case evaluation.
All information you share with our New Jersey nursing home abuse attorneys at our affiliate law firms remains confidential through an attorney-client relationship.
Resources:
 Hudson County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
Hudson County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
