legal resources necessary to hold negligent facilities accountable.
Las Vegas Nursing Home Abuse Lawyer
 Elderly residents in nursing homes are frequently subjected to various forms of abuse and neglect, leading to severe physical and emotional distress. This widespread problem indicates a systemic failure in providing safe and compassionate care to the elderly.
Elderly residents in nursing homes are frequently subjected to various forms of abuse and neglect, leading to severe physical and emotional distress. This widespread problem indicates a systemic failure in providing safe and compassionate care to the elderly.
Nursing Home Law Center, LLC's nursing home abuse attorneys are committed to confronting these injustices head-on. We strive to provide effective legal solutions that compensate victims and drive improvements in nursing home care standards.
Las Vegas Nursing Home Abuse Lawyer: Protecting the Rights and Dignity of SeniorsAbuse and neglect are pressing issues in Las Vegas, often overshadowed by the city's glitz and glamour. At its core, the role of a nursing home abuse lawyer is to safeguard the dignity and rights of our most vulnerable citizens – the elderly. Our law firm is dedicated to providing legal assistance to abused or neglected victims, ensuring their voices are heard and their rights are protected.
Nursing homes should be safe havens for the elderly, yet instances of nursing home neglect and abuse are alarmingly common. This abuse can manifest in various forms, including the following:
- Physical Abuse: This encompasses injuries such as bruises, cuts, or broken bones. These injuries are often unexplained or given inconsistent explanations by staff members.
- Emotional Abuse: Indicators include signs of depression, withdrawal, or fear. These symptoms are particularly alarming when they become apparent in the presence of certain staff members or other residents, pointing towards emotional mistreatment.
- Sexual Assault: This is marked by indications of non-consensual sexual contact. Evidence can include physical signs or abrupt changes in behavior, highlighting a severe breach of personal safety and dignity.
- Financial Abuse: This type manifests through unexplained withdrawals from bank accounts, changes in wills, or the disappearance of personal belongings.
- Neglect: Signs of neglect are visible through poor hygiene, malnutrition, or untreated medical conditions. These symptoms indicate a failure to provide adequate care, often due to negligence or medical malpractice.
Las Vegas's burgeoning senior population has unfortunately led to an increase in nursing home abuse cases. The city, known for its vibrant lifestyle and entertainment, is also home to numerous nursing facilities where elder abuse can occur. Recognizing the magnitude of this problem is the first step in combating it.
Elder neglect and abuse are not just isolated incidents but a systemic issue within many caregiving facilities. The prevalence of such cases in Las Vegas nursing homes has necessitated a stronger legal stance against these injustices. It's crucial to understand that these are not mere statistics; they represent real people suffering from emotional and physical injuries.
Rising Concerns in a Growing Senior PopulationNevada's demographic shifts have increased the senior population, placing additional strain on nursing facilities. This growth has, unfortunately, corresponded with a rise in abuse incidents. Understanding these demographic changes is critical to addressing the issue effectively.
As the elderly population grows, so does the demand for eldercare facilities. However, this increased demand can sometimes lead to compromised care standards, resulting in nursing home neglect. Addressing these rising concerns involves legal intervention and a societal commitment to the well-being of our elderly.
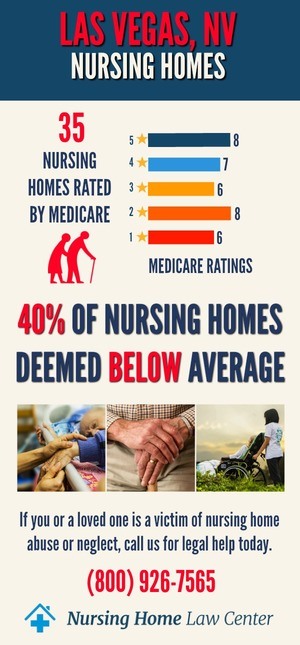
CMS Nursing Home Statistics in Las Vegas, NevadaThe Centers for Medicare and Medicaid Services (CMS) January 2024 revealed concerning statistics regarding Las Vegas, Nevada nursing facilities. Out of the 42 facilities assessed, a notable 14, representing 33% of the total, received ratings categorized as "below average" or "much below average." These ratings indicate the potential quality of care issues within a significant portion of Las Vegas nursing facilities.
Furthermore, inspectors have cited specific facilities for instances of abuse, emphasizing the need for thorough investigations and interventions to protect resident safety. The following facilities have been cited for abuse:
- El Jen Skilled Care
- North Las Vegas Care Center
- Royal Springs Healthcare and Rehab
These statistics underscore the importance of vigilance and advocacy to protect nursing home residents. The resident's family should stay informed about the quality of care in these facilities and take appropriate action if they suspect neglect or abuse.
Defining Abuse and Neglect in Elder CareIn the realm of nursing home abuse, it's essential to define what constitutes abuse and neglect. These terms encompass a range of harmful behaviors, from intentional physical abuse to more subtle forms of emotional distress and neglect. Understanding these definitions is crucial for family members and legal professionals alike.
Abusive behavior in nursing homes includes any action that harms or puts an elderly resident at risk. This can range from physical violence to emotional manipulation, financial exploitation, or inadequate care. Conversely, neglect involves failing to provide necessary care, leading to harm or a significant risk of harm.
Identifying Signs of Abuse and NeglectRecognizing the signs of nursing home abuse and neglect is a critical first step in safeguarding the welfare of elderly patients. These signs can be physical, emotional, or behavioral, and recognizing them can be the difference between continued suffering and timely intervention.
Visible signs of physical abuse in nursing homes include bruises, cuts, or other unexplained injuries. Sexual abuse also leaves physical evidence, along with profound emotional trauma. Emotional indicators, though less tangible, are equally significant and can manifest as fear, anxiety, or depression.
Subtle Signs of Neglect and AbuseLas Vegas nursing home neglect can be harder to detect than outright abuse. Signs of neglect include the following:
- Poor hygiene
- Malnutrition
- Developing bed sores
Behavioral changes, such as withdrawal or agitation, can also indicate neglect or abuse, necessitating a closer examination of the care provided.
Legal Protections Against Nursing Home AbuseThe legal system offers numerous protections against mistreatment. These laws are designed to uphold patient rights and dignity, ensuring they receive the care and respect they deserve. Understanding these legal protections is vital for victims and their families.
Federal and Nevada Nursing Home LawsFederal and state laws in Nevada provide a framework for protecting nursing home residents. These laws set standards for nursing facility care, ensuring that residents are treated with dignity and respect. Familiarity with these laws is crucial for anyone looking to understand or address mistreatment.
Reporting Nursing Home AbuseWhen suspecting nursing facility abuse, knowing how to report it is crucial. Timely reporting is essential in stopping abuse and initiating legal action against those responsible.
Families can also file a formal complaint to the following agencies:
- Disability Services Division
- Nevada Division of Public and Behavioral Health
- Nevada State Long-Term Care (LTC) Ombudsman Program
Personal injury attorneys are vital in addressing the issue of elder abuse. They provide legal representation, support, and advocacy for victims and their families, ensuring that justice is served and compensation is secured for the wrongs committed.
Attorneys specializing in nursing home abuse provide crucial support to victims and their families. They help navigate the complex legal landscape, from gathering medical records to filing a personal injury claim.
Seeking Justice and CompensationFiling a nursing home abuse claim involves seeking compensation for damages such as:
- Medical expenses
- Pain and suffering
- In tragic cases, funeral expenses
- Punitive damages in cases of severe abuse or neglect
Nursing home abuse lawyers guide victims through the process of obtaining just compensation, offering legal support when justice is sought for the abused and neglected.
Navigating the Challenges of Nursing Home CasesNursing abuse cases can be complex and challenging, requiring specialized legal expertise. From gathering evidence to understanding the nuances of Nevada law, these cases demand a thorough and professional approach.
Overcoming Obstacles in Evidence GatheringOne of the primary challenges in nursing abuse cases is gathering sufficient evidence. This process can be complicated, given the vulnerability of the victims and the nature of the abuse. Attorneys play a crucial role in overcoming these obstacles, ensuring the evidence is collected effectively and ethically.
In Las Vegas, nursing home abuse claims must be filed within a specific time frame, as dictated by the statute of limitations. Understanding these time limits is essential for timely legal action; attorneys can guide clients in navigating these deadlines.
Choosing the Right Las Vegas Nursing Home Abuse LawyerSelecting the right nursing facility abuse lawyer is critical for victims and their families. The right attorney will have the expertise, compassion, and commitment to navigate these challenging cases successfully.
Las Vegas Expertise in Elder Abuse LawChoosing a law firm with expertise in elder abuse law is imperative when dealing with nursing home negligence. An experienced nursing facility abuse lawyer will comprehensively understand federal and state regulations governing nursing facilities. Such expertise is vital in ensuring that the legal rights of elderly family members who have suffered abuse are fully protected.
Choosing a law firm with a dedicated team of nursing home abuse lawyers and elder abuse attorneys is crucial. Our attorneys are well-versed in the intricate aspects of eldercare facility laws and bring empathy and understanding to each case. This empathetic approach is fundamental when families have to confront the reality that their elderly loved ones have been subjected to emotional trauma or mental harm within a care facility.
Compassionate Legal SupportAbused victims and their families need more than just legal advice; they require compassionate support. Our law firm offers a free consultation to discuss the possibility of filing a wrongful death lawsuit or a wrongful death claim in the case of fatal abuse.
We stand ready to provide free case evaluation and represent clients on a contingency fee basis, ensuring that elderly loved ones receive the justice they deserve without upfront legal fees.
Legal Proficiency in Elder Care Facility CasesNavigating the complexities of personal injury cases within assisted living facilities requires a nuanced understanding of state and federal law. As such, our attorneys are meticulous in ensuring that every aspect of the law is adhered to, whether it pertains to the following:
- Rehabilitation center
- Nursing home facility
- Elder care home
Our firm's expertise and dedication to justice offer a beacon of hope for those who have suffered abuse and are seeking to hold the responsible parties accountable.
Hiring a Las Vegas Nursing Home Lawyer to Resolve Your Compensation ClaimDo you suspect nursing home abuse injured your loved one? At Nursing Home Law Center, LLC, we understand how distressing this can be. Call our nursing home abuse lawyers today at (800) 926-7565 for a free legal consultation to help you understand your rights and determine the best course of action.
Our expert legal team offers a free, no-obligation consultation, providing the support and guidance you need. We work on a contingency fee agreement, meaning we only get paid if we win your case.
 Clark County Nursing Home Injury Lawyer Nursing Home Law Center LLC Home
Clark County Nursing Home Injury Lawyer Nursing Home Law Center LLC Home