legal resources necessary to hold negligent facilities accountable.
Elgin Nursing Home Abuse Lawyer
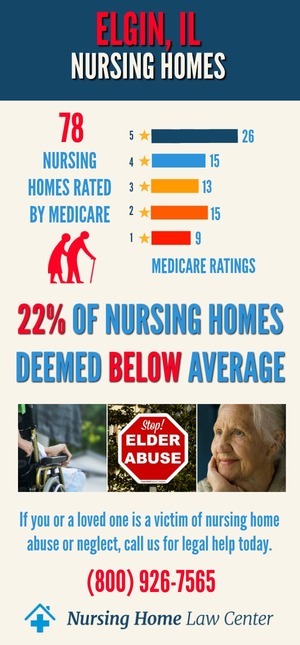 Elder abuse in nursing homes is a significant yet often overlooked problem, resulting in harm to some of the most defenseless individuals. This abuse can escalate to severe injury or even lead to premature death, exacerbating the vulnerability of nursing home residents.
Elder abuse in nursing homes is a significant yet often overlooked problem, resulting in harm to some of the most defenseless individuals. This abuse can escalate to severe injury or even lead to premature death, exacerbating the vulnerability of nursing home residents.
Nursing Home Law Center, LLC's nursing home abuse attorneys are dedicated to confronting this grave issue. We provide comprehensive legal services to victims, working relentlessly to secure justice and appropriate compensation.
The Gravity of Nursing Home Abuse in ElginNursing Home Law Center, LLC, as a dedicated Elgin nursing home abuse lawyer, understands the profound impact of abusive behavior on families and their elderly loved ones. In Elgin, the unfortunate reality of such abuse has become a pressing concern, warranting legal intervention.
The prevalence of nursing facility abuse underscores the need for specialized legal representation, which our firm is committed to providing with empathy and expertise. Our firm specializes in defending the rights and dignity of disabled and elderly residents, offering a beacon of hope and justice.
We are resolute in our mission to address these abuses and protect the most vulnerable members of our community, leveraging our extensive experience in personal injury cases. Each situation of suffered nursing home abuse is met with a tailored approach, ensuring that every nursing home resident receives the dedicated legal support they deserve.
Nursing Home Statistics in Elgin, IllinoisThe Centers for Medicare and Medicaid Services (CMS) January 2024 assessment findings indicate a concerning situation where 52 out of the 136 facilities assessed, representing 38% of the total, received ratings categorized as "below average" or "much below average" by CMS.
Facilities Cited for AbuseSome nursing facilities with below-average ratings faced additional scrutiny from inspectors who identified instances of mistreatment. The following Elgin, Illinois, nursing homes were cited for abuse:
- Aperion Care Hillside
- Aperion Care West Chicago
- Alden Valley Ridge Rehab & Healthcare Center
- Bella Terra Bloomingdale
- Citadel of Glenview
- Downers Grove Rehab & Nursing
- Elevate Care Niles
- Elevate Care North Branch
- Forest View Rehab & Nursing Center
- Generations Oakton Pavilion
- Grove of Elmhurst
- Hearthstone Manor
- Inverness Health & Rehab
- Lutheran Home for the Aged
- Meadowbrook Manor - Naperville
- River View Rehab Center
- Wealshire Center of Excellence
The spectrum of nursing facility abuse encompasses various forms, each detrimental to the well-being of nursing home residents. As an Elgin nursing home abuse lawyer, our firm confronts these realities daily, witnessing firsthand the devastating effects on individuals and families.
Abuse in caregiving homes ranges from physical and emotional trauma to financial exploitation and sexual abuse, leaving lasting scars on victims. Our nursing home abuse legal team is deeply committed to bringing these injustices to light and providing a path to healing and restitution.
Prevalence and Types of AbuseAbuse in nursing homes manifests in various forms, each causing significant harm to patients.
- Physical abuse involves direct harm to the body
- Emotional abuse encompasses mental and psychological distress
Financial exploitation and sexual abuse are also prevalent, violating the trust and safety of elderly loved ones. Our nursing home abuse lawyers are well-versed in identifying and addressing these abuse types, ensuring that victims receive justice and fair compensation.
Identifying Signs of AbuseRecognizing the signs of nursing facility abuse is crucial for timely intervention. Physical indicators, such as unexplained injuries, and behavioral changes, like withdrawal or fear, can be telltale signs. Financial irregularities may also suggest exploitation.
- Physical Abuse: The presence of injuries like bruises, cuts, or broken bones, mainly when explanations from staff are absent or inconsistent, making the caregiving home liable for personal injury.
- Emotional Abuse: Symptoms such as depression, withdrawal, or fear, especially noticeable near specific staff or patients, could suggest emotional harm due to a lack of proper care.
- Sexual Abuse: Any evidence of non-consensual sexual contact, whether physical or behavioral, requires immediate attention, as it points to serious violations within the nursing home facilities.
- Financial Abuse: Unexplained financial transactions or changes in personal legal documents might implicate the facility in financial abuse, with law firms often providing free case consultation to assess such situations.
- Neglect: Observable lack of care, including poor hygiene, malnutrition, or untreated health conditions, could be construed as medical negligence, warranting a detailed free consultation.
- Medical Malpractice: When substandard medical care leads to injuries or exacerbates health issues, it can constitute medical malpractice. Victims and their families may be entitled to compensation for suffering, pain, and other damages.
Our Elgin elder abuse attorneys are skilled in discerning these signs, aiding families in understanding and responding effectively to potential abuse scenarios.
Legal Framework and Resident RightsThe legal landscape governing abusive behavior is complex, with specific statutes and regulations in place to protect patients. As experienced injury lawyers, our firm navigates these laws, advocating for the rights and safety of nursing home residents.
Understanding and enforcing these legal protections are central to our practice, ensuring nursing facilities are held accountable for mistreatment.
Illinois Law on Elderly AbuseState law provides a clear framework for addressing abusive behavior and defining and penalizing various forms of mistreatment. Each Elgin nursing home abuse lawyer at our law firm is proficient in these laws, applying them effectively to protect patients and seek justice for wrongdoings.
Residents' Rights and ProtectionsResidents' rights in caregiver homes include the right to safe, respectful, and dignified treatment. Our legal team ensures that these rights are upheld, advocating for patients who have suffered abuse or neglect.
Families and employees can hold the nursing home liable for mistreatment by reporting abuse or neglect by contacting any of the following agencies:
- Illinois Department of Public Health
- Illinois Adult Protective Services
- National Center on Elder Abuse
Choosing our nursing home abuse attorneys means partnering with a team deeply committed to justice and client well-being. Our expertise in nursing home abuse cases sets us apart, ensuring each client receives personalized and effective legal representation.
Expertise and ExperienceOur lawyers bring a wealth of experience and specialized knowledge in nursing home abuse cases, making us a trusted choice for families seeking justice and fair compensation for their loved ones.
Client-Centric ApproachOur nursing home abuse lawyer team prioritizes each client's unique needs and circumstances, offering compassionate and tailored legal representation. Our approach concerns our clients' and their families' well-being and rights.
Addressing Systemic IssuesWe engage in legal actions that target systemic issues in caregiver homes, aiming to foster safer patient environments. Our advocacy focuses on upholding high standards of care and accountability.
Advocacy and Community EngagementOur involvement in community and advocacy efforts reflects our dedication to improving senior care home standards and promoting awareness of abusive behavior.
Hiring Our Nursing Home Abuse Lawyers to Protect Your Loved OneNursing Home Law Center, LLC lawyers are staunch advocates for disabled and elderly patients. Contact our nursing home abuse lawyers at (800) 926-7565 to schedule a free case evaluation for compassionate and competent legal aid.
We provide:
- Skilled personal injury lawyers addressing caregiving home negligence
- Assistance with nursing home neglect and elder law matters
- Legal support for cases of verbal abuse and wrongful death in caregiver homes
We uphold the legal obligation to protect the elderly, ensuring legal action leads to results.
 Cook County Nursing Home Injury Lawyer Nursing Home Law Center LLC Home
Cook County Nursing Home Injury Lawyer Nursing Home Law Center LLC Home
