legal resources necessary to hold negligent facilities accountable.
Chula Vista Nursing Home Abuse Lawyer
 Nursing residents often face various forms of abuse and mistreatment, including inadequate care, physical abuse, and emotional neglect. This abuse not only violates their rights but also endangers their health and well-being.
Nursing residents often face various forms of abuse and mistreatment, including inadequate care, physical abuse, and emotional neglect. This abuse not only violates their rights but also endangers their health and well-being.
At Nursing Home Law Center, LLC, we specialize in representing neglected and abused victims. Our Chula Vista nursing home abuse lawyers are dedicated to helping families achieve justice and secure the best possible outcomes for their loved ones.
Legal Protections for Chula Vista's Elderly ResidentsIn Chula Vista, it's essential to recognize the vulnerability of elderly patients and the importance of maintaining a safe, nurturing environment. Instances of nursing home neglect and abuse not only undermine their fundamental rights but also call into question the integrity of nursing homes and assisted living facilities.
The issue of nursing home abuse in San Diego County, and specifically in Chula Vista, highlights a need for awareness and proactive measures. Understanding the different forms of abuse, recognizing the signs, and knowing the legal steps to take are vital for protecting our elderly loved ones.
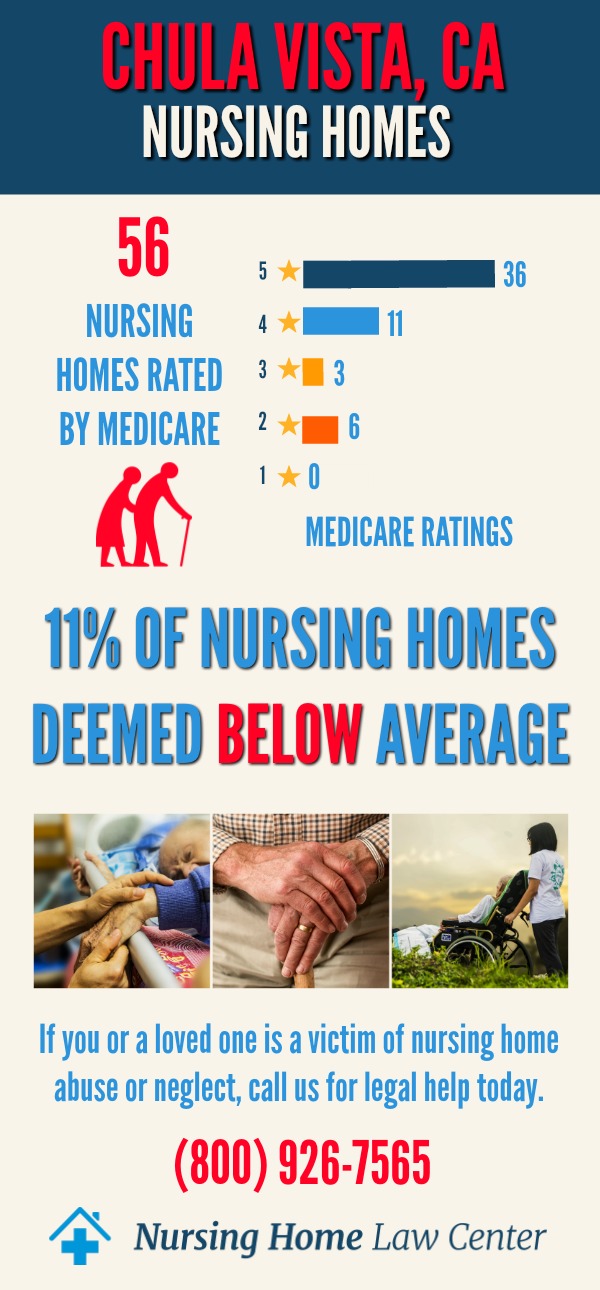
Nursing Facility Care Quality Concerns in Chula VistaRecent data from the Centers for Medicare and Medicaid Services (CMS) in December 2023 reveals that in Chula Vista, California, a notable 17% of nursing homes, amounting to 14 out of 81 facilities, have an overall rating as "below average" or "much below average."
This statistic raises significant concerns about these Chula Vista facilities' standard of care and oversight, emphasizing the need for enhanced quality control and monitoring to ensure the well-being and safety of elderly residents in Chula Vista.
Types of Nursing Home Neglect and AbuseAbusive behavior in Chula Vista encompasses a range of harmful behaviors that can lead to severe harm and even wrongful death. Understanding the types of nursing home abuse is the first step toward prevention and legal redress.
- Physical Abuse: This form of mistreatment involves any physical harm inflicted upon nursing residents. It can range from minor injuries to more severe harm, profoundly impacting the well-being of elderly patients.
- Sexual Abuse: Unwanted sexual contact with elderly residents in nursing homes is a deeply violating form of abuse. Recognizing the psychological and physical impact of sexual abuse is essential in providing the necessary support and taking legal steps.
- Mental Abuse: Psychological and emotional trauma inflicted upon nursing patients can have long-lasting effects on their mental health.
- Neglect: Failing to provide primary care, including medical, nutritional, and personal care needs, leads to significant health risks and deterioration in nursing residents.
- Financial Abuse: Exploitation of the monetary resources of nursing patients includes unauthorized use of their funds or assets, often leading to significant financial loss and vulnerability.
- Medical Malpractice: Negligence or improper medical treatment by a nursing home staff member can result in serious health complications or a preventable death, necessitating legal accountability and proper care standards.
Recognizing the signs of abuse and neglect is a critical step in safeguarding the well-being of elderly residents. Here are key indicators to watch for:
- Physical Indicators: Unexplained injuries like bruises or fractures in nursing homes and assisted living facilities.
- Behavioral Changes: Withdrawal, agitation, or other sudden mood shifts.
- Living Conditions: Poor conditions or inadequate staffing suggest neglect.
- Unexplained Symptoms: Sudden weight loss and mood changes hinting at potential abuse or neglect.
Vigilance in monitoring the condition and treatment of nursing home residents is critical to identifying and preventing abuse. Family members and visitors should be aware of the common warning signs of elderly mistreatment.
The Steps to Take After Suspecting Abuse in Nursing HomesIf you suspect that a family member or loved one is a victim of Chula Vista nursing home abuse or neglect, immediate action is required. This includes documenting the signs of abuse, speaking with the victim if possible, and seeking legal advice from a qualified nursing home abuse lawyer.
Report Nursing Home Neglect and Abuse to the Proper AuthoritiesTo effectively address negligence, mistreatment, or abuse in a nursing care facility, it's crucial to understand the steps involved and their importance.
- Reporting Abuse: It's imperative to promptly alert authorities, such as the Ombudsman, to initiate protective measures for residents.
- Legal Action: Engaging a specialized attorney can provide the necessary expertise for navigating legal complexities.
- Evidence Collection: Amassing detailed evidence, from medical documentation to witness testimonies, is foundational for building a strong case.
- Documentation and Expert Testimony: These elements are indispensable in lending credibility and weight to the abuse allegations.
- Settlements and Trials: Navigating these legal avenues demands the understanding and experience of a seasoned lawyer.
- Legal Advocacy: Neglect attorneys specializing in elder abuse serve as legal representatives and staunch champions for the rights of vulnerable seniors.
Resources for reporting abuse include:
- California Adult Protective Services
- California Advocates for Nursing Home Reform (CANHR).
- California Department of Public Health's Licensing and Certification Division
- California Long Term Care Ombudsman Program at (800) 231-4024.
- Division of Medi-Cal Fraud & Elder Abuse (DMFEA): (800) 722-0432.
- Elder and Dependent Adult Abuse Reporting Hotline: (888) 436-3600.
A Chula Vista nursing home abuse lawyer can play a vital role in addressing instances of abuse and neglect, such as:
- Physical abuse
- Sexual abuse
- Financial abuse
- Negligence
From providing legal representation to navigating the complex legal system, these professionals are equipped to advocate effectively for victims and their families.
Remove Victims From Harmful Situations and Seek CompensationDeveloping strategies to safely remove Chula Vista nursing facility victims from abusive situations and seeking fair compensation for the harm suffered are key roles of a nursing home abuse attorney.
Seeking compensation is a critical aspect of the legal process for victims of nursing facility abuse and neglect. This not only addresses the financial impact of the abuse but also serves as a form of justice for the victims and their families.
Identifying Liable Parties in Chula Vista Nursing Home Abuse CasesIdentifying the liable parties in nursing abuse civil cases is crucial. This may include individual caregivers, nursing facility administrators, or the facility itself, depending on the circumstances of the abuse.
Victims of nursing home abuse and their families may be entitled to various forms of compensation, including the following:
- Medical expenses
- Pain and suffering
- Funeral and burial expenses in wrongful death cases
A nursing home abuse lawyer can help determine the appropriate compensation based on the case's specifics.
Hire a Chula Vista Nursing Home Abuse Lawyer to Resolve a Compensation ClaimExperiencing bodily harm demands compassionate counsel and aggressive representation. Our lawyers at Nursing Home Law Center, LLC will pursue justice for your family member on a contingency fee agreement, ensuring those responsible are held accountable. Reach our nursing home abuse lawyers at (800) 926-7565 for a free consultation.
 San Diego County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
San Diego County Nursing Home Injury Attorney Nursing Home Law Center LLC Home
